Case Report - (2023) Volume 8, Issue 2
Volumetric modulated arc therapy of a jugulo-tympanic paraganglioma: a case with a literature review
Received Date: Jan 30, 2023 / Accepted Date: Feb 06, 2023 / Published Date: Feb 15, 2023
Abstract
Paragangliomas are neuroendocrine tumors originating from the extra-adrenal paraganglia of the autonomic nervous system. Most paragangliomas of the cervico-facial region are benign and slow growing, but 10% may have metastasis [1]. Jugulotympanic location represent the second most common tumor of the temporal bone. Treatment options for patients with head and neck paragangliomas include surgery, normofractionated external cortical radiation therapy (RT), stereotactic radiation therapy (SRS) or observation. The vital prognosis is good, but the functional prognosis remains critical especially for large tumors.
Keywords
Paragangliomas, Neuroendocrine Tumors, Radiation Therapy
Introduction
Paragangliomas are benign tumors that arise from the paraganglionic system. The most common symptoms of tympanicjugular paragangliomas are pulsatile tinnitus and conductive hearing loss. All patients undergo MRI of the head and neck, CT bone scanning, bilateral carotid angio-graphy and catecholamine screening.The most frequently used classification is that of Fisch [2], and the treatment is guided by this classification. The best treatment when feasible is total surgical removal, with or without preoperative embolization. Otherwise subtotal removal, with or without postoperative radiotherapy is also an option, or partial resection or primary radiotherapy for symptomatic tumor. We can also wait and monitoring by using CT for asymptomatic patients [3]. This case report present the role of Volumetric modulated arc therapy in ttreatment of tympano-jugular paraganglioma, and discusses current recommendations from the literature.
Case Presentation
A 60-year-old female patient, with no past medical history, presented to the hospital for bilateral hearing loss and dysphonia that started 1 year ago and got worse. The otoscopic examination revealed a pulsatile retro tympanic vascular mass. Head and neck MRI revealed Expansive process centered on the right jugular gulf with T1 hypersignal, T2 heterogeneous hypersignal and flair with a typical salt and pepper aspect .this process measure 28*20*27mm in diameter.
Topographically it enlarges the homolateral jugular and hypoglossal foramina, posteriorly and medially, comes into contact with the cerebellar pontine angle without any sign of invasion, inferiorly and anteriorly occupies the retrostylial parapharyngeal space and comes into contact with the internal carotid artery.
The MRI appearance was in favor of right tympanic jugular paraganglioma type D1 according to the Fisch classification, with invasion of the hypoglossal foramen complicated by atrophy of the hemi-larynx and attraction of the hemi-larynx to the left side (Figure 1).
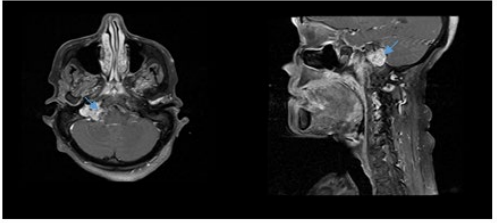
Figure 1: Axial and sagittal T1-weighted Gadolinium enhanced MRI showing hypersignal contrast enhancing lesion involving tympanojugular région (blue arrow).
The patient was surgically recused and sent to radiotherapy department, radiation was scheduled as soon as possible and delivered dose was 54 Gy with 2Gy per fraction. The patient was surgically recused and sent to radiotherapy department, radiation was scheduled as soon as possible and delivered dose was 54 Gy with 2Gy per fraction.
For planning radiation treatment, we used CT simulator (Siemens, Erlangen, Germany). The gross tumor volume (GTV) was contoured in MRI and adjusted on the planning CT. For CTV, 5-mm margin was given around GTV to have high-risk CTV (CTV-HR), and was adjusted on the planning CT to restricted natural barriers such as bone and air. CTV was expanded by isotropic 5 mm margin to generate planning target volume (PTV). The dose prescription was 54 Gy at 2 Gy per fraction. OARs (cord, brainstem, optic chiasm, right optic nerve, and cochleae…) were contoured (Figure 2&3).
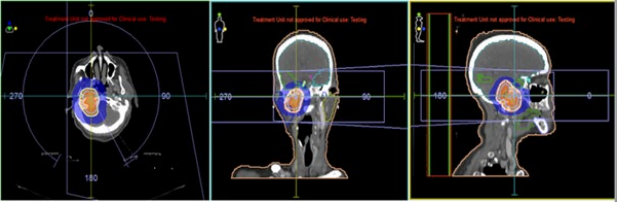
Figure 2: Different views of the planning computed tomography scan showing the target volumes: GTV in red, CTV-HR and PTV-HR in purple and blue, respectively. Volumetric modulated arc therapy was delivered to the region of high risk, to doses of 54 Gy (95% isodose line in blue).
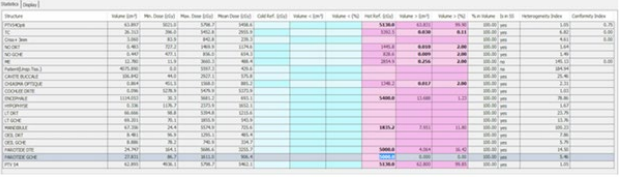

Figure 3: Dose-volume histogram distribution of the following structures. planning target volume,optic chiasm,optic nerves,mandible,spinal cord,brainstem,right cochlea,right pituitary,right parotid gland.
One arc volumetric modulated arc therapy (VMAT) plan with 6-MV photon beams was set by the medical physicist. Planning goals for the PTV based on ICRU 83 were the following: at least 90% and 95% of the prescribed total do (PTD) encompassing at least 98% and 95% of PTV, respectively (V≥ 98% and V≥ 95%, respectively); and no more than 2% of PTV received more than 107% of the PTD (V ≤ 2%).
The following constraints were set for some OARs: for cord, the maximum dose received by 2% of its volume less than 45 Gy (D2% < 45 Gy); for brainstem, D2%< 55 Gy; for optic chiasm, D2%< 60 Gy; for temporal lobes, D2% < 65 Gy; lastly, the mean dose received by right cochleae 53,73Gy (Table 1).
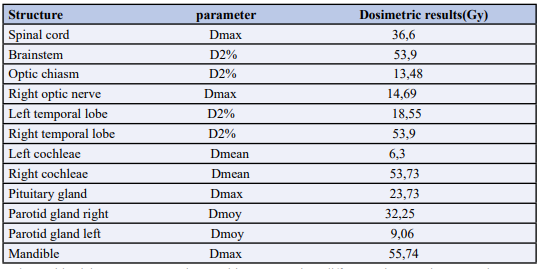
Table 1: Main dosimetric results for organs-at-risk.
VMAT plan was done with Elekta Versa HD. Patient position was verified weekly by kV cone beam CT imaging prior to treatment. The patient tolerated the treatment and was seen weekly during treatment by our doctors. No significant side effects were observed except otalgia and grade 1 skin réaction. After radiotherapy completion, the patient was clinically evaluated every 3 months, and after 6 months we noted a regression of tumor volume from 28*20*27 mm to 19*15*18 mm.
Discussion
Paragangliomas are benign tumors that arise from the paraganglionic system. They represent 0.03% of all neoplasia and 0.6% of head and neck tumors [4-5]. Jugular and tympanic paragangliomas are the most common tumors of the middle ear. They represent 18- 36% of the para-gangliomas of the cervico-facial region; 60-80% are carotid paragangliomas and 3-4% are vagal paragangliomas. There is no racial predilection, but females are 4-6 times more affected than males. The most frequent symptom is a pulsatile tinnitus, present in 80% of cases. In 60% of the cases, we find a hearing deficit, of transmission or of perception depending to the location and extension of the tumor [6]. Hearing loss is found in 52% to 91% of cases [7,8]. Audiometry is essential. It specifies the type of hearing loss, conductive in the less advanced forms, or mixed, of variable degree. Baguley et al. [9] show a proportional relationship between sensory involvement and tumor size.
The diagnosis of paraganglioma is based on clinical and radiological aspects based on CT, MRI and arteriography in order to support the diagnosis and clarify the tumor extension. The different therapeutic strategies are very diverse and controversial. The treatment of these tumors is surgical for most authors [10,11]. Indeed, surgical resection allows a complete and definitive treatment, especially since the sequelae in the tympanic forms are most often acceptable (mainly unilateral hypoacusis), unlike the jugular forms where neurological sequelae with cranial nerve damage predominate.
Radiotherapy has little place in the treatment of pure tympanic forms where surgery must be proposed as first line, with acceptable risks of sequelae.Although this attitude is not unanimous, according to some authors [12], it is indicated for very large tumors that recur after treatment,and when tumor persist after surgery.
The dose necessary and sufficient to control this benign and slowly evolving tumor seems to be between 40 and 50 Gy [13,14] administered in 25 fractions spread over 5 days per week.This dose avoid acute and late toxicities, in particular temporal necrosis and osteoradionecrosis, while ensuring a good local control. It is therefore a compromise between efficacy and tolerance: below 40 Gy, relapses are observed [15], whereas above 50 Gy, the rate does not appear to be higher.
Due to the proximity of target volume to radiosensitive normal structures, they might be good candidate for advanced radiotherapy technologies, such as intensity-modulated radiation therapy (IMRT) or volumetric modulated arc therapy (VMAT) because of their high accuracy and ability to deliver higher radiation doses to the tumor and to spare surrounding tissues.
The indication for stereotactic radiotherapy is becoming common, for example in the case of bilateral lesions for which surgical resection is done at the risk of bilateral neurological deficits, with serious functional sequelae. Stereotactic radiotherapy is also indicated in cases of incomplete surgical resection, non-operated tumors, due to invasion of the internal carotid artery, for example, in cases of recurrence, or in elderly patients or those unable to tolerate the operative risks.The most recent data in the literature show that Gamma Knife, LINAC and/or Cyberknife achieve a very good tumor and symptom control rate ranging from 71% to 100% and 88% to 100% respectively, with a much lower morbidity than surgery [16-17]. Some transient effects are noted such as facial paresis and headache.However, it should be emphasized that this stereotactic irradiation modality only concerns Paragangliomas of less than 3 cm in diameter, residual or recurrent after surgery. Moreover, fractionated irradiation delivering low doses in 30 sessions equivalent to a single dose of 15-16 Gy seems interesting for giant inoperable Paragangliomas [18].
Chemotherapy is not part of the classical therapeutic arsenal for paragangliomas of the head and neck, nor for other localizations. Treatment with Iodine-131-MIBG, which aims at destroying by Iodine-131 electively the cells that capture MIBG, allows a very high selectivity of the therapeutic action. Its effectiveness would be encouraging
Conclusion
Surgery in paragangliomas has long been the treatment of choice, but the sequelae on the cranial nerves and the risk of bleeding make it controversial today.Radiotherapy constitutes today an effective treatment of jugular paragangliomas. Intensity modulated conformal radiotherapy or VMAT can allow a progressive control of the tumor in 90 to 99% of cases with a low risk of minor complications. It has become the first-line choice.
Conflict of Interest Statement
The authors declare no conflicts of interest
References
1. Williams MD (2017) Paragangliomas of the head and neck: an overview from diagnosis to genetics. Head and Neck Pathology 11(3):278-287. 2. Fisch U (1982) Infratemporal fossa approach for glomus tumors of the temporal bone. Ann Otol Rhinol Laryngol 91:474-479.
3. Offergeld C, Brase C, Yaremchuk S, Mader I, Rischke HC, et al. (2011) Head and neck paragangliomas. Head Neck 33:1530-1534.
4. https://umbalk.org/wp-content/uploads/2020/05/20. TYMPANOJUGULAR-PARAGANGLIOMAS.pdf
5. Roger Christian, Meva’a Biouélé & Djomou, François & Zoe, Cathy & Honga, Vanina & Dalil, et al. (2016). Trois cas de paragangliome tympanojugulaire observés au Cameroun. African J Pathol Microbiology 5:1-4.
6. Remley KB, Coit WE, Harnsberger HR, Smoker WR, Jacobs JM, et al. (1990) Pulsatile tinnitus and the vascular tympanic membrane : CT, MR, and angiographic findings. Radiology 174:383-389.
7. Brown JS (1985) Glomus jugular tumor revised: a ten year statistical follow-up of 231 cases. Laryngoscope 95:284-288.
8. Alford B, Guilford FR (1962) A comprehensive study of tumors of the glomus jugulare. Laryngoscope 72:765-787.
9. Baguley DM, Irwing RM, Hardy DG, Harada T, Moffat DA (1994) Audi-ological findings in glomus tumours. Br J Audiol 28:291-297
10. Jackson CG (2001) Glomus tympanicum and glomus jugulare tumors. Otolaryngol Clin North Am 34:941-970.
11. Duet M, Sauvaget E, Guichard JP, Petelle B, Ledjedel S, et al. (2002) Scintigraphy by octreos- can in the management of head and neck paragangliomas. Ann Otolaryngol Chir Cervicofac 119:315-321.
12. Hinerman RW, Mendenhall WM, Amdur RJ, Stringer SP, Antonelli PJ (2001) Definitive radiotherapie in the management of chemodectomas arising in the temporal bone, carotid body, and glomus vagale. Head Neck 23:363-371.
13. Kim JA, Elkon D, Lim ML, Constable WC (1980) Optimumdoseofradiotherapyforchemodecto- mas of the middle ear. Int J Radiat Oncol Biol Phys 6:815-819.
14. Wang CC (1980) What is the optimum dose of radiation therapy for glomus tumors? Int J Radiat Oncol Biol Phys 6:945-946.
15. Larner JM, Hahn SS, Spaulding CA, Constable WC (1992) Glomus jugulare tumors. Long-term control by radiation therapy. Cancer 69:1813-1817.
16. Pollock BE (2004) Stereotactic radiosurgery in patients with glomus jugulare tumors. Neurosurg Focus 17:E10.
17. Lee CC, Pan DH, Wu JC, Chung WY, Wu HM, et al. (2011) Gamma knife radiosurgery for glomus jugulare and tympanicum. Stereotact Funct Neurosurg 89:291-298.
18. Minniti G, Clarke E, Cavallo L, Osti MF, Esposito V, et al. (2004) Fractionatedstereotacticconformalradio- therapy in the management of large chemodectomas of the skull base. Int Radiat Oncol Biol Phys 58:1445-1450.
Copyright: © 2025 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.



