Case Report - (2023) Volume 8, Issue 1
Subtotal esophagectomy with esophagogastroplasty after esophageal perforation and stent insertion: Case report of a challenging situation
Received Date: Dec 27, 2022 / Accepted Date: Jan 01, 2023 / Published Date: Jan 31, 2023
Abstract
We present a case of failure of uncovered metal esophageal stent removal, which was inserted after iatrogenic esophageal perforation during endoscopy. A 58-year-old male patient presented with dysphagia, chest pain, globus sensation and vomiting. Based on the data of the performed preoperative studies and to avoid the possibility of developing fatal complications (primarily aortoesophageal fistula) the surgical intervention was recommended. The successful subtotal esophagectomy with immediate esophagogastroplasty was then performed. The control X-Ray examination was performed at 6th p/o day, which reveals no extravasation and free passage of contrast to the distal part of GI tract. The patient started peroral eating and was discharged the Hospital at 7th p/o day. We consider, that this surgical procedure seems to be the most optimal and radical surgical intervention in case of failed esophageal stent placement.
Keywords
Esophageal Stent, Subtotal Esophagectomy, Esophagogastroplasty
Introduction
Iatrogenic esophageal perforation after endoscopy or surgery is a severe and potentially life-threatening condition, which requires rapid diagnosis and immediate appropriate treatment. For decades, surgical intervention and drainage procedures were the standard methods of treatment for benign esophageal perforation. More recently, various endoscopic therapies, including different esophageal stents insertion have been introduced in clinical practice [7-12,14,15]. The possibility of using of an esophageal endoprosthesis was first described in 1845 and the first successful experience was described by G. Symonds in 1887 using prostheses made of ivory and silver [1,2,14]. At the present time, esophageal stent placement is utilized for a wide variety of different benign and malignant esophageal pathologies. A variety of esophageal stents (metal, plastic, or biodegradable) are currently available in 3 types: uncovered, fully covered, and partially covered. The most common indication for an esophageal stent placement remains palliation of malignant dysphagia and another indication, other than dysphagia, is esophageal leakage or perforation. However, this seemingly effective and safe procedure does not rule out the development of different complications, which can occur in early and delayed post procedure period and may be life-threatening. Herein, we describe and discuss a case of delayed complication of failed stent placement after iatrogenic esophageal perforation during endoscopy.
Case Report
A 58-year-old male patient presented with dysphagia, chest pain, globus sensation and vomiting. From his medical history it became known that a 1 year ago at the Hospital in another country during endoscopic examination he underwent pneumocardial dilation procedure, during which the iatrogenic damage to the esophagus occurred. Due to the developed mediastinitis and exudative pleurisy, the patient was transferred to the ICU department and systemic antibiotic therapy, parenteral nutrition, mediastinal and pleural drainage and subsequently the esophageal stenting with uncovered metal stent was performed. Performed clinical, laboratory and instrumental studies revealed the following clinical picture (Figure 1 and 2). Taking into account the above complaints, the data of the performed studies and the possibility of developing fatal complications (primarily aortoesophageal fistula) the surgical intervention was recommended.
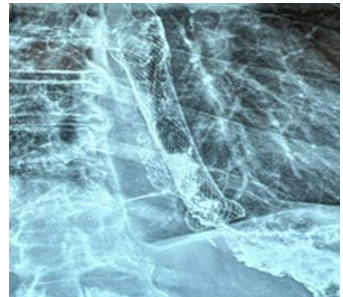
Figure 1: Preoperative X-Ray Data.
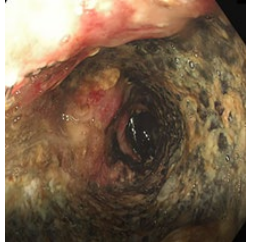
Figure 2: Preoperative Endoscopy View.
Operative Treatment
At 15.XII.22 Subtotal Esophagectomy with Immediate Esophagogastroplasty was performed. At laparotomy the mobilization of stomach and abdominal segment of esophagus was performed. At subsequent thoracotomy mobilization of thoracic part of esophagus and gastric tube formation was performed and esophagogastric anastomosis was created (Figure 3-5). The most difficult and dangerous part of operation was the dissection and mobilization of thoracic part of the esophagus due to severe adhesions in the mediastinum and pleural cavity, pronounced peri esophagitis and dense adhesions of the esophagus with the aorta. Insertion of nasojejunal tube and drainage of pleural and left subdiaphragmatic spaces completed the operation. Undoubtedly, an important role for the success of a complex and major operation is played by adequate anesthesia. This part of the surgical intervention was performed as follows. Anesthesia plan: induction was made with dexmedetomidine 0.5 mcg/kg, propofol 2.0 mg/kg, rocuronium 0.7 mg/kg, lidocaine 0.5 mg/kg and dexamethasone 4 mg. Intubation was done with double lumen tube 37 Fr size, to separate right lung. Epidural catheter was placed at level of T6-T7 and 8 ml of 0,125% bupivacaine was given continuously for pain management.
Maintenance of anesthesia: Target-controlled infection was maintained for sedation and analgesia with propofol 1% 4mg/ kg/h and dexmedetomidine 0,7 mcg/kg/h. Multi modal opioid free anesthesia technique was done, which provides excellent anesthesia and analgesia. For monitoring was used invasive arterial blood pressure and invasive venous blood pressure to guide safety hemodynamic parameters. During operation several times arterial blood gas test has been done to control oxygenation parameters. After operation patient was extubated in operation room and with safety guidance transferred in ICU for overnight treatment.
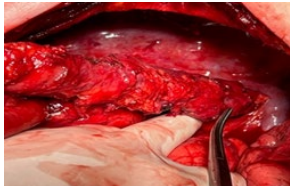
Figure 3: Mobilization of thoracic part of esophagus
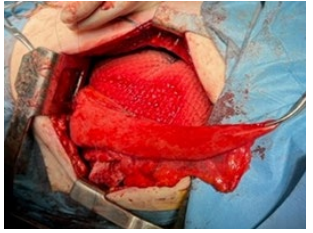
Figure 4: Gastric tube creation
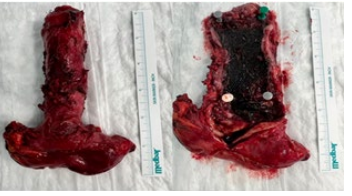
Figure 5: Surgical Specimen with Stent inside.
Results
Postoperative course was uneventful and without complications. The control X-Ray examination was performed at 6th p/o day, which reveals no extravasation and free passage of contrast to the distal part of GI tract. The patient started peroral eating and was discharged the Hospital at 7th p/o day. At control X-Ray and Endoscopy examination after 1 month of surgery the patient is doing well, eats semi-liquid food and does not show any special complaints (Figure 6 and 7).
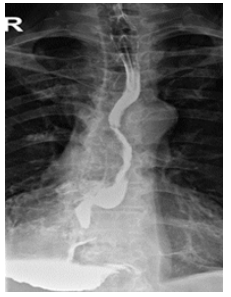
Figure 6: Control X-Ray after 1 month of surgery
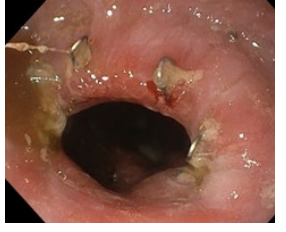
Figure 7: Endoscopic view after 1 month of surgery.
Discussion
ESGE recommends that temporary stent placement can be considered for treating esophageal leaks, fistulas, and perforations. The optimal stenting duration remains unclear and should be individualized [16]. Stent-related complications can be divided onto two groups: early and delayed complications. Early complications occur immediately or within 1-month post procedure and include: chest pain, fever, bleeding, gastroesophageal reflux disease, globus sensation, perforation, and stent migration. Early complications were reported in up to 32% of patients. Delayed complications, which are present months after the procedure include: tumor ingrowth, stent migration, stent occlusion, development of esophageal fistulae, and recurrence of strictures. Delayed complications have been reported in 53-65% of patients, with a reintervention rate of up to 50% [3,17]. T. Järvinen et al. reported stent complication rates between 23% and 56%, with an overall stent failure rate of 34.3% [4]. Another group of authors concluded that failure rates are higher than described in the literature [5,13,15]. Furthermore, H. Iwasaki et al. reported that mortality rate associated with esophageal stent placement varied from 3.9% to 27.2% [6]. The most serious and dangerous complication is developing of gastroaortic or aortoesophageal fistula, which could lead to fatal outcome. So, many authors have concluded that esophageal stenting carries out significant risk of various complications, which requires the different additional minor and major interventions [3-5,13,15,18-20]. Our case, which is described above, fully confirms this assumption.
Conclusion
Our case illustrates, that esophageal stenting is not as simple and safe procedure as described in the literature, which could lead to very serious complications and challenging problems.
Esophageal stenting in patients with esophageal perforation should be performed only for the minimum necessary period and stent-related complications can be prevented by removal of the prosthesis as soon as possible after insertion.
In case of failure of esophageal stent removal, presence of different complications with possibility of aortoesophageal fistula formation the best results can be achieved by resective surgical treatment and subtotal esophagectomy with immediate esophagogastroplasty seems to be the most optimal surgical intervention. These patients should be under close outpatient monitoring for early diagnosis of developing complications and determination of the most optimal immediate treatment method.
References
1. D’Etiolles L, De Lavacherie De l’Oesophagotomie 1845 (Bruxelles).
2. Symonds CJ (1887) The treatment of malignant stricture of the oesophagus by tubage or permanent catheterism. Br Med J 1:870-873.
3. Hindy P, Hong J, Lam-Tsai Y, Gress F (2012) A Comprehensive Review of Esophageal Stents. Gastroenterol Hepatol (NY) 8(8):526-534.
4. JärvinenT, Ilonen I, Kauppi J, Rasanen J (2019) Esophageal stent failure: a retrospective cohort study. Annals of Esophagus 2:10:
5. Glatz T, Marjanovic G, Kulemann B, Hipp J, Theodor Hopt U, et al. (2017) Management and outcome of esophageal stenting for spontaneous esophageal perforations. Diseases of the Esophagus 30:1-6.
6. Iwasaki H, Mizushima T, Suzuki Y, Fukusada S, Kachi K, et al. (2017) Factors That Affect Stent-Related Complications in Patients with Malignant Obstruction of the Esophagus or Gastric Cardia. Gut Liver 11(1):47-54.
7. Freeman RK, Van Woerkom JM, Ascioti AJ (2007) Esophageal stent placement for the treatment of iatrogenic intrathoracic esophageal perforation. Ann Thorac Surg 83(6):2003-2007.
8. van Heel NC, Haringsma J, Spaander MC, Bruno MJ, Kuipers EJ (2010) Short-Term Esophageal Stenting in the Management of Benign Perforations. American Journal of Gastroenterology 105(7):1515-1520.
9. Van Heel NC, Haringsma J, Spaander, MC, Kuipers EJ (2009) Complications of Long-Term Esophageal Stenting in the Management of Benign Perforations. Gastrointestinal Endoscopy 69(5):123-124.
10. Khaitan PG, Famiglietti A, Watson TJ (2022) The Etiology, Diagnosis, and Management of Esophageal Perforation. J Gastrointest Surg 26(12):2606-2615.
11. Smoliar AN, Radchenko Iu A, Nefedova GA, Abakumov MM (2014) Esophageal stenting complications. Khirurgiia (Mosk) (12):29-35.
12. Thornblade LW, Cheng AM, Wood DE, Mulligan MS, Saunders MD, et al. (2017) A Nationwide Rise in the Use of Stents for Benign Esophageal Perforation. Ann Thorac Surg 104:227-233.
13. Wang MQ, Sze DY, Wang ZP, Wang ZQ, Gao YA, et al. (2001) Delayed complications after esophageal stent placement for treatment of malignant esophageal obstructions and esophagorespiratory fistulas. J Vasc Interv Radiol 12(4):465- 74.
14. Ong GKB, Freeman RK (2017) Endoscopic management of esophageal leaks. J Thorac Dis. 2017 9(2):S135-S145.
15. Vermeulen BD, Siersema PD (2018) Esophageal Stenting in Clinical Practice: An Overview. Curr Treat Options Gastroenterol (2):260-273.
16. Spaander MC, Baron TH, Siersema PD, Fuccio L, Schumacher B, et al. (2016) Esophageal stenting for benign and malignant disease: European Society of Gastrointestinal Endoscopy (ESGE) Clinical Guideline (2016). Endoscopy 48(10):939- 948.
17. Homann N, Noftz MR, Klingenberg-Noftz RD, Ludwig D (2008) Delayed complications after placement of selfexpanding stents in malignant esophageal obstruction: treatment strategies and survival rate. Dig Dis Sci 53(2):334- 40.
18. Chikinev IU V (2015) Extirpation of Esophagus after Stenting. Vestnik Exp Clin Surg VIII:1 2015:87-91
19. Sugumar A, Baron TH (2009) Causes for Reintervention After Esophageal Stent Placement: A Single Center Experience. GIE 69:352.
20. McManus K, Khan I, McGuigan J (2001) Self-expanding oesophageal stents: strategies for re-intervention. Endoscopy 33(7):601-604.
Copyright: © 2025 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.



