Case Report - (2023) Volume 8, Issue 1
Pituitary carcinoma: A rare presentation
Received Date: Feb 12, 2022 / Published Date: Feb 01, 2023
Abstract
Pituitary carcinoma (PC) is a very rare feature of pituitary tumors, which is defined by the presence of cerebrospinal and/or systemic metastases. These tumors pose a problem of diagnosis and management. Multimodal therapeutic strategy include surgery, radiotherapy and chemotherapy has improved the poor prognosis of these patients.
We present the case of a 50-year-old patient, diagnosed with pituitary carcinoma, surgically recused, who received exclusive radiation therapy.
Keywords
Pituitary, Carcinoma, Radiotherapy
Introduction
Pituitary carcinoma are epithelial tumor of the pituitary gland, with an incidence of 0.1 to 0.2% of pituitary tumors [1]. The revealing clinical presentation depends on the functional or non-functional character of the tumor, as well as the size and extent of the tumor. Metastases are rarely present at the time of diagnosis, they appear of a variable period after the initial diagnosis. Surgical resection is the principle of treatment. Radiotherapy as a local treatment increases local control in case of incomplete resection or in case of non-resecable tumor. Systemic treatment can control symptoms of hypersecretion in relation to remote metastases.
Case Presentation
This is a 50-year-old patient, without any particular medicalsurgical antecedents, who has for four months rapidly progressive headaches of moderate intensity, with the appearance of a decrease in bilateral visual acuity.
A brain scan and angio-MRI requested by his ophthalmologist showed a sellar process of 37*34*28 mm, encompassing optic chiasma, infiltrates the posterior ethmoidal cells and extends to the base of the skull above (Figure 1).
The patient has benefited from an endosanal biopsy revealing a pituitary carcinoma. Given the extent of the tumor, carcinological surgery was not feasible.
The patient received exclusive external radiation therapy. The administered dose was 50.4 Gy in 1.8 Gy/fraction (Figure 2). The processing took place without incident.
An evaluation scanner performed three months after the end of treatment showed a lesion stability at the local level, a multiple bilateral cervical lymphadenopathy, with metastatic localisation in the liver bone and lymph nodes.
The patient was referred to medical oncology for palliative chemotherapy, but unfortunately died before treatment.
Discussion
Pituitary tumors are dominated by pituitary adenomas. The association of these tumors with an invasion of the dura, bone or vessels defined invasive pituitary adenomas [2,3]; the term of which may lead to confusion with pituitary carcinomas. These carcinomas are defined only by the presence of craniospinal and/ or systemic metastases [4].
Pituitary carcinoma are very rare tumors with an incidence of 0.1 to 0.2% of pituitary tumors [1]. They can develop in both sexes with a 1:1 sex ratio, and at any age but typically presents in the third to fifth decade of life, at a mean age of 44 years. Several studies reported latency periods vary from 4 months to 18 yr, with a mean interval of 7 years [5].
Most pituitary carcinomas are diagnosed as invasive macroadenoma. In addition, more than two thirds of these tumors are hormonally active, with hormonal hypersecretion tables mimicking pituitary adenomas. The most common endocrine syndromes are Cushing’s disease (42%) and hyperprolactinemia (33%), followed much less commonly by acromegaly (6%) and hyperthyroidism (1%) [6].
For endocrinologically non-functional tumors, representing 15- 20% of these tumors, the clinical signs are those of a tumor mass syndrome, most often with headaches and visual disorders.
Non-central nervous system metastasis are the most common, the most affected sites are the liver, bone and cervical lymph nodes [7]. In the central nervous system, series reported the involved of the cerebral cortex, cerebellum, spinal cord, leptomeninges, and dura [8,9].
MRI is the reference radiological exam for the sellar region analysis [10]. The most radiological aspect is that of an invasive macroadenoma. The intrasellar component exhibits aggressive and destructive behavior with supra and parasellar extension, with possible invasion of the cavernous sinus. MRI can also visualize possible metastases in the central nervous system. These metastases have the same radiological characteristics of the intrasellar tumor [11].
Radionuclide and functional imaging studies using specific radiotracers have also been employed to better study the extent of the primary lesion and metastases. These include meta-iodobenzylguanidine (MIBG), octreotide (111In-pentreotide) [12,13], dopamine D2-receptor ligands (123I-epidepride) [14], and tumor metabolites (18F-deoxyglucose; 11C-L-methionine) [15] scintigraphy scans.
The management of pituitary carcinoma poses a real challenging because of the rarity of this pathology. The different therapeutic modalities are essentially surgery, radiotherapy, chemotherapy and hormonal manipulation.
Because of the presence of metastases at the time of diagnosis, carcinological surgery of the primary tumor is often not indicated. The place of surgery can be discussed in the case of metastases of the central nervous system, such as the case of a single symptomatic brain metastasis, a nodule subarachnoid compressing the spinal cord, the cerebral parenchyma or the base of the skull. For systemic metastases, the possibility of resection of vertebral, hepatic or even pulmonary lesions is still poorly defined and rarely practised by surgeons.
Radiotherapy remains an important part of the treatment of pituitary adenomas. Nevertheless, for proven pituitary carcinomas, radiation therapy does not seem to change the natural history of this pathology [16]. In two-thirds of cases, patients with pituitary carcinoma had a prior irradiation of pituitary adenoma. Radiotherapy on central nervous system metastases can help stop tumor proliferation, and even induce a partial remission. It can also be discussed in patients surgically recused [17], but without scientific evidence on its effectiveness [18]. Irradiation of bone metastases and more rarely visceral metastases was also applied to improve local control.
Stereotactic radiotherapy or cyber-knife have the advantage of irradiating small tumor volumes close to the organs at risk, and thus reduce the risk of radiation-induced damage [19]. These more sophisticated irradiation techniques allow a re-irradiation of patients already irradiated by conventional techniques developing metastases or recurrences [19].
Several cytotoxic agents have been used for pituitary carcinomas, including cisplatin, carboplatin, etoposide, adriamycin, dacarbazine, cyclophosphamide, procarbazine, vincristine, mitotane, and methotrexate. However, given the rarity of this condition no randomized trial has evaluated the benefit of any of these drugs.
Recently two protocols are the most administered were cyclohexyl-chloroethyl-nitrosourea (CCNU) in combination with 5-fluorouracil (5FU), this combination was chosen because it had some activity against systemic neuroendocrine tumors. Temozolamide is indicated in patients with pituitary carcinoma resistant to standard therapy; it has approved an efficacy of about 37%, especially with functioning tumors [20].
Hormonal treatment by may be beneficial in some symptomatic patients with a functional tumor, but in the majority of cases these patients have already received this type of treatment with hormonal escape.
Conclusion
Pituitary carcinoma is a rare and aggressive condition. Several modalities have been proposed in the majority of cases for a palliative purpose. A better knowledge of the molecular behavior and pathogenesis of these tumors can contribute to the development of new therapies to improve the prognosis of these patients.
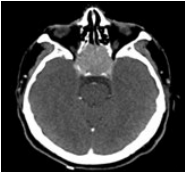
Figure 1: Axial section of cerebral CT showing the tumor process.
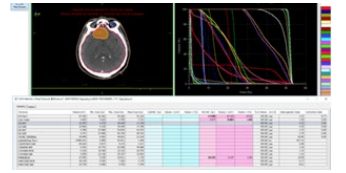
Figure 2: Target volume and dose volume hitogram.
References
1. Faehndrich J, Weidauer S, Pilatus U, Oszvald A, Zanella FE, et al. (2011) Neuroradiological viewpoint on the diagnostics of space-occupying brain lesions. Clin Neuroradiol 21(3):123- 139.
2. Ragel BT, Couldwell WT (2004) Pituitary carcinoma: a review of the literature. Neurosurg Focus 16:E7.
3. Ironside JW (2003) Best practice no 172: pituitary gland pathology. J Clin Pathol 56:561–568.
4. Kaltsas GA, Grossman AB (1998) Malignant pituitary tumours. Pituitary 1:69-81.
5. Roncaroli F, Scheithauer BW, Horvath E, Erickson D, Tam CK, et al. (2010) Silent subtype 3 carcinoma of the pituitary: a case report. Neuropathol Appl Neurobiol 36:90-94.
6. Ragel BT, Couldwell WT (2004) Neurosurg. Focus 16:E7.
7. Kaltsas GA, Grossman AB (1998) Pituitary 1:69-81.
8. Holthouse DJ, Robbins PD, Kahler R, Knuckey N, Pullan P (2001) Corticotroph pituitary carcinoma: case report and literature review Endocr. Pathol 12:329-341.
9. Tysome J. Gnanalingham K, Chopra I, Mendoza N (2004) Intradural metastatic spinal cord compression from ACTHsecreting pituitary carcinoma. Acta Neurochir. 146:1251- 1254.
10. Thapar K, Laws ER Jr. (2001) In: Brain tumors: an encyclopedic approach. 2nd ed. Kaye, A. H. and Laws, E. R. Jr. (eds.). Churchill Livingstone: London.
11. Tsuki M, Kaji Y, Matsuo M (2000) MR findings of subarachnoid dissemination of a pituitary adenoma. Br J Radiol 73:783-785.
12. Greenman Y, Woolf P, Coniglio J, O’Mara R, Pei L, et al. (1996) Remission of acromegaly caused by pituitary carcinoma after surgical excision of growth hormone-secreting metastasis detected by 111-indium pentetreotide scan. J Clin Endocrinol Metab 81:1628-1633.
13. Dayan C, Guilding T, Hearing S, Thomas P, Nelson R, et al. (1996) Biochemical cure of recurrent acromegaly by resection of cervical spinal canal metastases. Clin. Endocrinol 44:597- 602.
14. Petrossians P, de Herder W, Kwekkeboom D, Lamberigts G, Stevenaert A, et al. (2000). Malignant prolactinoma discovered by D2 receptor imaging. J Clin. Endocrinol Metab.85:398-401.
15. Muhr C, Bergstrom M, Lundberg PO, et al. (1988) Malignant prolactinoma with multiple intracranial metastases studied with positron emission tomography. Neurosurgery 22:374- 379.
16. McCutcheon IE, Pieper DR, Fuller GN, Benjamin RS, Friend KE, et al. (2000) Pituitary carcinoma containing gonadotropins: treatment by radical excision and cytotoxic chemotherapy: case report. Neurosurgery 46:1233-1240.
17. Wilson DF (1982) Pituitary carcinoma occurring as middle ear tumor. Otolaryngol Head Neck Surg 90:665-666.
18. Ragel BT, Couldwell WT (2004) Pituitary carcinoma: a review of the literature. Neurosurg Focus 16:E7.
19. Swords FM, Allan CA, Plowman PN, Sibtain A, Evanson J, et al. (2003) Stereotactic radiosurgery. XVI. A treatment for previously irradiated pituitary adenomas. J Clin Endocrinol Metab 88:5334-5340.
20. Mccormack A, Dekkers OM, Petersenn S, Popovic V, Trouillas J, et al. (2018) Treatment of aggressive pituitary tumours and carcinomas: Results of a European society of endocrinology (ESE) survey 2016. Eur J Endocrinol 178(3):265-276.
Copyright: © 2025 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.



