Case Report - (2022) Volume 7, Issue 11
Periodontal regeneration after third molar extraction causing attachment loss in distal and furcation sites of the second molar: a case report with 12 months follow-up
2Center for Interdisciplinary Research in Health, Portugal
3Department of Surgery and Periodontology, Centro Universitário Newton Paiva, Brasil
4Department of Periodontics and Oral Medicine, University of Michigan School of Dentistry, Ann Arbor, USA
Received Date: Nov 02, 2022 / Accepted Date: Nov 08, 2022 / Published Date: Nov 20, 2022
Abstract
Introduction: The periodontal support apparatus is extremely important due to guarantee insertion to the tooth. It helps with the maintenance of the structural resistance and reconstructive property, and its loss may contribute to root exposure and the possibility to obtain an augmentation of the sensitivity. Thereby, this paper aimed to describe a case report, using regenerative techniques in a bone loss involving distal and furcation regions of the mandibular second molar, which was associated with the extraction of the adjacent impacted third molar without bone interposing.
Case presentation: The patient was referred to a private dental clinic reporting an unpleasant odor while using dental floss in the distal region of the mandibular left second molar, during the three years. In addition, reported a history of extraction of the wisdom tooth six years ago. Periapical examination and periodontal index were performed and an extensive radiolucent image involving distal and furcation regions, with a 12 mm probing depth involving the distal root at tooth (2nd molar). No other region showed probing depth greater than 3mm. Thus, after rigorous scaling and root planing, periodontal guided tissue regeneration was performed as an attempt to fill the bone defect.
Conclusion: The regenerative process is a predictable way to treat vital mandibular second molar after extraction of the adjacent third molar. Clinicians must give special attention to extraction involving the mandibular third molars, mainly when there is no bone interposed between the second and third molars.
Keywords
Bone Regeneration, Guided Bone Regeneration, Guided Tissue Regeneration, Osseous Defects, Osseous Surgery, Periodontal Regeneration, Periodontal Surgery
Introduction
Recurrent pericoronitis, orthodontic treatment, presence of associated pathologies, food impaction, periodontal involvement, and root resorption next to the second molar, are justificative for third molar extraction [1,2]. Pell and Gregory’s classification is one of the greater references to help in the diagnosis and surgical planning, which uses the space between the distal of the second molar and the ramus of the mandible as references to classify dental impaction (classes I, II, or III), also making a subdivision (A,B, and C) regarding the position of the third molar in relation to the occlusal plane [3].
Some complications resulting from the extraction of third molars are trismus, infectious processes, alveolar osteitis, swelling, hematomas, oroantral fistula, mandible fracture, paresthesia, osteomyelitis, and osteonecrosis [4,5]. These complications are notably known in scientific literature and usually help the clinician to plan and execute a procedure. However, few studies have investigated the healing process of an extracted third molar alveolus in cases they are in position B or C, without the presence of bone interposed between second and third molars.
Consequently, the periodontal support tissue is compromised and a great exposition of the root can occur leads to a decreased resistance and reparative property, increased possibility of sensitivity, and bacterial accumulation [6]. New formation and reinsertion of the periodontal ligament in areas that have experienced loss and root exposure are extremely difficult. The main cause that inhibits the new formation and insertion of ligament fibers is the high-speed proliferation of junctional epithelium in comparison to the bone, cement, and periodontal ligament6. Then, regeneration of the lost tissues is a concern in the clinical management of periodontal tissues in order to restore the periodontal apparatus and avoid tooth loss.
Thus, the objective of this paper was to describe a case report of the periodontal regeneration of bone loss involving distal and furca region of mandibular second molar which was boosted by extraction of the adjacent wisdom tooth.
Clinical Presentation
Diagnosis
Male, 28 years old, systemically healthy, and without relevant habits, reporting no family history of periodontal disease. The patient was referred to a private clinic reporting an unpleasant odor while using dental floss and no sensitivity in the distal region of the mandibular left second molar (#18), observed for three years. Moreover, the patient reported a history of tooth extraction (#17), six years ago, due to dental impaction classified as II-B, according to Pell and Gregory’s classification, with consequent pericoronitis.
The periapical radiograph showed an extensive radiolucent image involving the distal root and the furcation area of the tooth (#18) (Figure 1). The periodontal index was performed with a UNC-15 probe and no probing depth was greater than 3mm after examination, except for the distal region of tooth 37, with 12 mm of probing depth, receiving the diagnosis of a healthy periodontium. Nabers probe was used to check the furcation area of tooth #18, and a significant 5 mm mark from the buccal surface was noted, grade 2 for furcation defect. Clinical examination evidenced satisfactory hygiene, with bleeding on probing of 8%, no visible dental calculus deposits, and plaque index of 12%. Periodontal guided tissue regenerative surgery was planned to fill the periodontal bone defect after 14 days of the initial therapy.
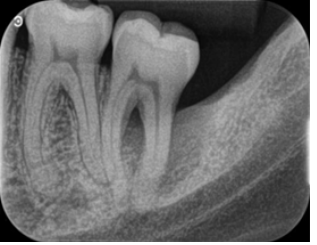
Figure 1: Extensive radiolucent image involving the distal root and the furcation area of the 2nd molar.
Case Management
Local anesthesia was performed using lidocaine 2% with epinephrine 1:100,000 . Intrasulcular incision with distal oblique extension and a full-thickness mucoperiosteal flap was made, showing the bone defect on the distal and buccal surfaces (Figure 2).
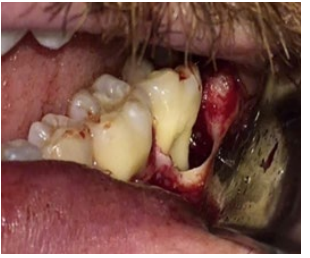
Figure 2: Periodontal bone loss on the distal and vestibular surfaces of the 2nd molar, after infra-bone granulation tissue removal.
Removal of the entire granulation tissue and mechanical treatment for decontamination of the exposed root surface was performed. Xenogenous bone graft substitute was used to fill the cavity (Figure 3). The resorbable membrane was used to prevent epithelial invagination between the dental surface and Bio-Oss® (Figure 4 A,B). The flap was repositioned and sutured with nylon suture (Figure 5).
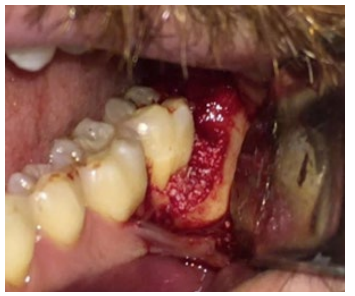
Figure 3: Xenogenous bone substitute was used to achieve osteoconduction.
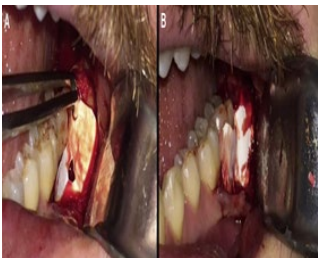
Figure 4: A) A resorbable membrane template; B) A resorbable membrane was used to prevent epithelial invagination, reaching the osteopromotion.
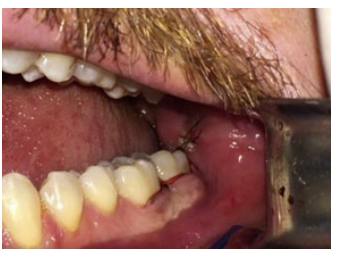
Figure 5: Flap repositioned and sutured with nylon suture thread.
Clinical Outcomes
The radiographic appearances before the surgical procedure, after three months, and twelve months after the surgery show the favorable and predictable result reached (Figure 6 A,B,C). Probing depth remained stable at 5 millimeters in the follow-up care consultations, after 3 and 12 months.
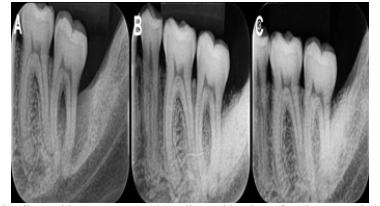
Figure 6: A) Pre-surgical initial radiographic appearance; B) Radiographic view after three months of the surgery; C) Radiographic appearance after twelve months of follow-up.
Discussion
Impacted third molar has 24.4% of prevalence, with mesioangular impaction as the most common (41.17%), followed by vertical impaction (25.55%), distoangular (12.17%), and horizontal (11.06%) [7]. It occurs 49% in men and 58% in women [8]. The II-C classification was the most common and it was found in 22% for tooth #17 and 24.5% for tooth 32 [8]. In our study, following the report given by the patient, it is believed that the impacted third molar previously extracted was in position II-B of the Pell and Gregory’s classification.
The involvement of the second molar was evaluated by Sun et al. [9]. The authors studied 1301 second molars of 457 patients and concluded that the removal of non-impacted third molars improves the patient’s periodontal condition [9]. On the other hand, impacted third molars, especially those in mesial inclination and C position, are significantly associated with greater destruction and resorption of adjacent second molar root [10].
Scientific literature addresses different surgical techniques for removing third molar and its consequences. Typically, they study the influence of the flaps, sutures, drug therapy, and biomaterials to fill the socket [11,12]. However, there is a lack of studies that describe detailed what occurs, after extraction, with the distal region of the second molar; what happens when the root surface is kept exposed; and whether the regenerate process is needed after wisdom extraction in order to minimize any negative outcome.
In this case report, the accessibility for oral hygiene was impaired due to having a deep root exposition, in a difficult region, and with furcation involvement. Thereby, it was planned scaling and root planing, followed by regenerative technique trying to reestablish the periodontal support tissue, obtaining an optimized result.
Conclusion
Within the limitation of this case report, it was possible to verify that the impacted third molar with the crown in contact with the anterior adjacent tooth (absence of bone interposed), may contribute, after removal, with root exposition and progression of a periodontal destructive feature. Thus, the regenerative technique can be employed and adopted, consciously, to fill and correct the bone defect, restoring the periodontal apparatus, with a stable result after 12 months.
Conclusion
1. Wang D, He X, Wang Y, Li Z, Zhu Y, et al. (2017) External root resorption of the second molar associated with mesially and horizontally impacted mandibular third molar: evidence from cone-beam computed tomography. Clin Oral Invest 21:1335-1342.
2. Sarica I, Derindag G, Kurtuldu E, Naralan M, Caglayan F (2019) A retrospective study: Do all impacted teeth cause pathology? Niger Journ Clin Pract 22(4):527-533.
3. Pell GJ, Gregory GT (1933) Impacted mandibular third molars: classification and modified techniques for removal. Dent Digest 39(9):330-338.
4. Giovacchini F, Paradiso D, Bensi C, Belli S, Lomurno G, et al. (2018) Association between third molar and mandibular angle fracture: A systematic review and meta-analysis. J Cran Max Fac Surg 46:558-565e.
5. Monteiro RJSV, Pereira AG, Olivo EAC, Moura MF, Costa FO, et al. (2016) Alveolar osteitis: risk factors and treatment modalities. Braz Journ Surg Clin Res 15(3):68-72.
6. de Jong T, Bakker AD, Everts V, Smit TH (2017) The intricate anatomy of the periodontal ligament and its development: Lessons for periodontal regeneration. J Periodont Res 52:965- 974.
7. Carter K, Worthington S (2016) Predictors of Third Molar Impaction: A Systematic Review and Meta-analysis. J Dent Res 95(3):267-276.
8. Cordero E, Vallejos D, Sadovnik I, Romo L (2011) Study of prevalence of third molar according to Pell and Gregory classification. Int J Oral Maxillofac Surg 40(10):1127.
9. Sun LJ, Qu HL, Tian Y, Bi CS, Zhang SY, et al. (2020) Impacts of non-impacted third molar removal on the periodontal condition of adjacent second molars. Oral Dis 26(5):1010- 1019.
10. Smailien D, Trakinien G, Beinorien A, Tutlien U (2019) Relationship between the Position of Impacted Third Molars and External Root Resorption of Adjacent Second Molars: A Retrospective CBCT Study. Medicina 55:305-316.
11. Carrasco-Labra A, Brignardello-Petersen R, Yanine N, Araya I, Guyatt G (2012) Secondary Versus Primary Closure Techniques for the Prevention of Postoperative Complications Following Removal of Impacted Mandibular Third Molars: A Systematic Review and Meta- Analysis of Randomized Controlled Trials. J Oral Maxillofac Surg 70:441-457e.
12. Barbato L, Kalemaj Z, Buti J, Baccini M, La Marcas M, et al. (2015) Effect of Surgical Intervention for Removal of Mandibular Third Molar on Periodontal Healing of Adjacent Mandibular Second Molar: A Systematic Review and Bayesian Network Meta-Analysis. J Periodontol 87(3):291-302.
Copyright: © 2025 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.



