Research Article - (2022) Volume 7, Issue 10
Peer pressure and social adjustment as predictive indicators of substance abuse among selected sample of psychiatric patients in a teaching hospital in south-west, Nigeria
Received Date: Oct 06, 2022 / Accepted Date: Oct 12, 2022 / Published Date: Oct 20, 2022
Copyright: Copyright: ©2022: Segun-Martins IO. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Segun-Martins IO, Dennis UD, Ilori OP (2022) Peer pressure and social adjustment as predictive indicators of substanceabuse among selected sample of psychiatric patients in a teaching hospital in south-west, Nigeria. Journal of Clinical Review & Case Reports 7(10):122-127.
Abstract
Substance abuse is a major public health challenge the world over. Adequate research connection has not been fully established between peer pressure and social adjustment as predictors of substance abuse particularly among psychiatric patient. Therefore, this study examined the roles of peer pressure and social adjustment in predicting perceived substance abuse among Psychiatric patients. Using cross-sectional survey design, 198 patients (Male=119; Female=79) participated in the study. Their ages ranged from 18-40 (M=28.45, SD=4.22). Instruments used were 10-item Peer Pressure Inventory (PPI), 45-item Social Adjustment Inventory (SA), and 10-item Drug Abuse Screening (DAS). Three hypotheses were formulated and tested. The result showed that, peer pressure (β=0.33; p<0.05 level of significance) and social adjustments (β=0.61;p<0.05 level of significance) were significant predictors of substance abuse among Psychiatric Patients. The result of the regression analysis showed that peer pressure (β=0.38,p<0.01) significantly predicted substance abuse, social adjustment (β=0.25,p<0.01) showed a significant relationship to substance abuse and the two variables jointly predicted substance abuse (F(2.198)=3.97,p<0.05). It was recommended that the health sector should engage in enlightenment campaign on the negative consequences of substance abuse among psychiatric patients.
Keywords
Peer pressure, Social adjustment, Substance abuse, Psychiatric patients
Introduction
Background to the Study
The current data from the Nigerian Drug Law Enforcement Agency (NDLEA) suggest that drug and substance abuse is an ever expanding problem and an estimated 29.4 million Nigerians are active drug abusers and this situation is recognized as a threat globally with serious effects on people’s health, security, socialeconomic and cultural welfare [1]. Research on adolescence have consistently shown that there is considerable prevalence of drug and substance use; with varying preference rates found for both overall and specific drug abuse [1-3]. In recent times, reports of the UNODC suggest that in Nigeria there is a 14.4% increase in prevalence of drug use and globally, eleven (11) million people engage in drug use [4]. Some of these commonly abused substances include tobacco, amphetamine, cocaine/crack, amphetamines, caffeine, nicotine, ethanol, benzodiazepines, opioids, γ-hydroxybutyric acid, glue, poppers, solvents, lysergic acid diethylamide, dimethyltryptamine, psilocybin, mescaline, marijuana, methylene-dioxy-methamphetamine [4]. The current patterns of psychoactive drug production, and its consumption coupled with the system with which it is administrated is rapidly changing with the use of advancement of technology such as drone supplies, email and electronic delivery [5]. Studies have reported that countries where the most rapid changes are occurring, often include large population settlement, countries like Nigeria and other developing nations like India, Brazil, Malaysia and Singapore as well as Latin America are often cited [6,7].
The provisions for the definition of substance abuse as put forward by World Health Organization Definition [8]. posit that harmful persistent administration of psychoactive substances, including but not limited to alcohol and illicit drugs. The WHO further added that cannabis and amphetamines remains the most sort-after illicit substance in the African region. Some authors have defined substance use as the excessive, maladaptive or addictive use of drugs for non-medical purpose that interferes with a healthy and productive life excessive, maladaptive or addictive use of drugs for non-medical purpose [9-12]. The American Psychological Association [13] define substance use disorder as the excessive use of psychoactive substance; that include alcohol, tobacco, opoids, and amphetamines that leads to impaired personal and social control, risky behaviour, tolerance to the drug and withdrawal symptoms.
Mental patients have often disclosed during intervention that the journey into substance use often originate as a result of social influence, especially those concerned with siblings, and peer relations that consequently lead to peer pressure [14]. Most people who end up as substance users often are particularly adolescents who are subject to environmental influence and social desirability of wanting to be liked by their peers so as to gain in-group favoritism [15]. Coping with trending societal values for young people often lead to problems associated with social maladjustment. Individuals ability to cope with standards, values and need of the society in order to be accepted. It can be referred to as the psychological process which involves coping with new standard and values [16]. Scholars and researchers in Psychology describe social adjustment as the degree of social and interpersonal relations and how it affects perceived reaction to the demand of environmental influence (Mamman 2014).
Statement of Problem
The use of illicit drug has been recognized as a global public health issue responsible for the large number of proportion of health care budget and expenditure. The health burden linked to substance is inestimable [8]. The persistency of drug related crime have been linked the prevalence substance use [1,17]. With the increase in out-of-school adolescents and unemployed young adults, there seems to be no signs of abating this problem anytime soon. The pervading effects of substance abuse in psychiatric populations posts a huge healthcare expenditure for families, government and other stakeholders. The far-reaching effect of physical and mental deterioration, cuts across family and social relationships, employment, education and quality of life [18,19]. In addition, studies that have examine the influence of social variables such as peer pressure and social adjustment have been research carried out abroad. However, studies in Nigeria have not given attention this subject matter deserves. Most studies in Nigerian often focus on non-clinical samples. This have led to scant literature in the subject matter especially in psychiatric populations The understanding and management of psychiatric populations offers ecological validity of the predisposing factors associated with substance use problems.
Objectives of the Study
The objectives of this study was to determine the extent to which peer pressure and social adjustment predict substance abuse among psychiatric patients of Ladoke Akintola University Teaching hospital, Osun state. Specifically, this study aims to accomplish the following:
1. To determine whether peer pressure would predict substance abuse.
2. To examine whether social adjustment would predict substance abuse among psychiatric patients
3. To evaluate the joint influence of peer pressure and social adjustment and how it would predict substance abuse among psychiatric patients.
Hypotheses
Based on the objectives of the study, the following hypothesis were formulated:
H1 : Peer group influence will significantly predict substance abuse among psychiatric patients in such a way that patients who score high on the measure of peer pressure will be report increase perception towards substance abuse.
H2 : Social adjustment will significantly predict substance abuse among psychiatric patients in such a way that patients who report significant levels of social adjustment will report lower scores on perceived substance abuse.
H3 : Peer group influence and social adjustment will jointly and significantly predict increased perception of substance abuse among psychiatric patients.
Method
Research Design
The research design adopted in this study was cross-sectional survey design, as it attempted to analyze data collected from representative sub-set (Psychiatric patients). There were two independent variables which are: Peer group influence and social adjustment and one dependent variable, substance abuse. Data on these variables were collected simultaneously through administration of questionnaire.
Participants
Participants of this study are made up of a sample of two hundred and ten (210) Patients sampled across psychiatry ward of the hospital. Both in and out patients who are diagnosed of substance abuse was used for the study. They comprised of 119 (60.3%) males and 79 (39.7%) females with an age range of 18-25years (10) (6%), 26-30years (85) (43%), and ages beyond 31years (101) (51%). With regards to their religious affiliation, (169) (85.7%) were Christians, and (29) (14.7%) were Muslims. The marital status of the participants showed that singles were Single (26) (7.1%), Married (52) (33.4%), Divorced (74) (37.5%), Widow (44) (22%).
Sampling and Sampling Techniques
Accidental sampling techniques was used to select study participants at Ladoke Akintola Teaching Hospital, Osogbo, whereby sample of substance abuse patients (both in and out patients) who verbally volunteered was used for the study.
Instruments
Relevant data were gathered through validated self-report questionnaire which comprised 4 sections (Sections A-D). Section A: Demographic information of the participants contained the socio-demographic information of the participants such as age, gender, marital status, educational qualification and religion. Section B: This comprised the Peer Group Inventory developed by Robert (1970). Peer group influence scale is a unidimensional ten item scale designed to measure the influence of peer group. All items of the PGI were structured on a 4-point Likert type scale (No influence=0, Little=1, Some what=2, A lot=3). Any participant scoring more than 0 was considered to be experiencing peer group influence. Items are scored from 0-3, all items are scored directly. Adamson and Babalola [20] reported a Cronbach’s alpha of .82. Sample items include “How strong is the influence from your friends to sturdy hard or to do your homework”, “How strong is the influence from your friends to smoke marijuana”. Higher scores indicate greater influence from peer group. Section C: Social Adjustment Inventory (SAI). Social adjustment was measured using a 45 item self-report social adjustment scale developed by Roma [21]. Social adjustment was developed to assess global adaptability of human to a particular environment. It is a unidimensional scale rated on a 5-point scale (1=not at all, 2=occasionally, 3 about half of the time, 4=most of the time, 5=all the time). Sample item include: “felt upset, worried or uncomfortable at work?”, “felt lonely and wished for companionship?”. Scoring: scores of social adjustment are added together, in general, higher scores indicate better social adjustment. Nwakaego [22] reported crouchback alpha reliability of 0.77. An overall adjustment score was obtained by summing the scores of all the items and dividing by the number of items actually answered. Section D: Drug Abuse Screening Instrument; Drug Abuse Screening Test (DAST) is a unidimensional scale developed by Skinner [23]. It was designed to measure drug abuse with a 10 item scale. The inventory was rated on a two-point scale (0=No, 1=Yes). Sample items include “Do you ever feel bad about your drug abuse?”, “Are you unable to stop abusing drug when you want to?” “Do you ever feel guilty about your drug intake?”. A score of 1 is given for each YES response, except for items 3 for which a No response is given a score of 1. In a heterogeneous Psychiatric patient population, most items have been shown to correlate at least moderately well with the total scale sores. Skinner reported a Cronbach alpha of 0.92. Adama [24] reported an internal consistency reliability of 0.88. The DAST total score is computed by summing all items that are endorsed in the direction of increased drug problems.
Procedure
A letter of introduction was obtained from the Department of Pure and Applied Psychology, Adekunle Ajasin University, AkungbaAkoko, Ondo State. Letter requesting for permission to carry out a research using the psychiatric patients was sent to the Chief Medical Teaching Hospital Oshogbo and necessary payment was made to the admin before the administration of questionnaire. Data was collected with the use of questionnaire. Each participant was assured of confidentiality and anonymity of their responses to the questionnaire and they were also informed that participation was purely voluntary and that they are of liberty to discontinue with the study whenever they feel uncomfortable. To further conceal the identity of the participants, they were informed not to indicate their names of any part of the questionnaire. The researcher administrated two hundred and ten questionnaires and one hundred and ninety-eight questionnaires were found analyzable for the study. Therefore, the study yielded a response rate of 88%. The questionnaires were distributed, only to participants that consented to participate in the study.
Data Analysis
Pearson Product Moment Correlation (PPMC) analysis was used to evaluate the type and interrelatedness of the variables in this study. However, hypotheses 1 and 2 were analyzed using two step multiple regression. Step 1 of the regression model involved the socio demographic variables. In step 2 of the regression model, the predictors (Peer group influence and social adjustments) were entered. All analysis was carried out using Statistical Package for Social Sciences version 22.
Results
Pearson Product Moment Correlation (PPMC) analysis was conducted to test the relationship among the variables of the study. The results are presented in Table 1.
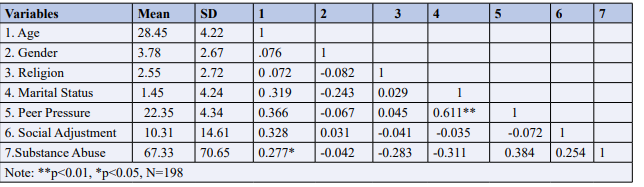
Table 1: Correlation Matrix Showing the Relationship Mean, Standard Deviation and the Relationship among the Study Variables
Results in Table 1 indicated that age had significant relationship with substance abuse (r=-0.27, p0.01) among psychiatric patients. This implies that patient’s gender difference had no significant relationship with perceived substance abuse among psychiatric patients. Religion showed inverse significant relationship with substance abuse (r=-0.28, p>0.05). This implies that as psychiatric patient’s religion increases, the lower the tendency of perceived substance abuse among psychiatric patients. Also, patient’s marital status showed significant inverse relationship with perceived substance abuse (r= -0.31, p>0.05). This implies that as student’s marital status increases the lower the inclination to engage in substance abuse among psychiatric patients. In addition, peer pressure showed significant relationship with perceived substance abuse among psychiatric patients (r=0.38, p>0.01). This implies that Peer Pressure showed significant influence on perceived substance abuse among psychiatric patients. Psychiatric patient’s social adjustment showed significant inverse relationship with substance abuse among psychiatric patients (r=0.25, p>0.01). This implies that as psychiatric patients’ perception of social adjustment increases, the lower the tendency for psychiatric patients to engage in the abuse of substance.
Test of Hypotheses
To test the study hypotheses a multiple regression analysis was conducted. The results are presented in Table 2.
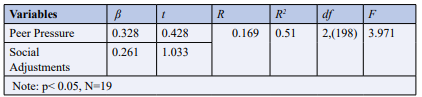
Table 2: Summary of Multiple Regression Analysis Showing the Predictive Influence of Peer Pressure and Social Adjustments on Substance Abuse.
Discussion
This study investigated the extent to which peer group influence and social adjustment predict substance abuse among psychiatric patients. This study tested three hypotheses and the results are discussed in this section. The first hypotheses which tested if peer pressure will significantly predict substance abuse among Psychiatric patients. Therefore, the result was confirmed. Peer pressure significantly predicts substance abuse. This confirmed the hypothesis and it was therefore accepted. One explanation for the outcome of this study, who found that the main reason that drug use and abuse often stems from influence within the environment and as a result it is a learned behaviour. Learned behaviour when reinforced often leads to habit forming proclivities. This position is similar to the findings by Kremer, (2008); Thakore, Ismail, Jarvis, Payne and Rothenburg [25]; Burke [26] who noted that perceived peer pressure was identified as a significant factor in youth development and impacts adolescents mostly. This is not far-fetched, in that, environment constitutes lots of individual with different behaviors and this gives people opportunity to meet different people from different background that can influence an individual positively or negatively through direct means or otherwise. Peer pressure may be the perpetuating factor in the spread of some behaviors that are not within some societal norms. In hypotheses two, which stated that social adjustment will significantly predict substance abuse among psychiatric patients was confirmed. Strawbridge [27] who noted that social adjustment does not in any way contribute to substance abuse. It is not surprising that there is divergent view in the previous empirical studies as related to social adjustment and substance abuse: this may be as a result of different views and attitudes that people hold to what constitute social adjustment and substance abuse. Hypotheses three stated that peer pressure, and social adjustment will jointly significantly predict substance abuse among Psychiatric patients was confirmed and accepted. Although there is quality of literature study in this area, but there is need for more studies as the rate of substance abuse recently is alarming. It is only logical to explain that, if the reward for abusing substance is substantial and rate of peer pressure is high, such individual will give reasons for his or her abuse of substances.
Conclusion
The study found that peer pressure was the major reason for substance abuse among patients. Patient under higher peer pressure are reported to make use of substance: this may be as a result of gaining peer acceptance and avoidance of negative feedbacks from peers, thus, matches their behaviors with perceived expectations from others. Also, it was noted that in this study, social adjustment and peer pressure exerted joint predictive influence on substance abuse. It is important for patients to consider the adverse effect of substance on themselves, their social consequences, and consequences on their interactions rather than considering the immediate and on the spot gratification the substance use may possess. Some of the adverse effect of abusing substance include but not limited to cognitive and social impairment, procrastination, risky sexual behaviors, criminal behaviors, and problems for care givers.
Recommendations
Based on the findings of this study, several recommendations were made to help address and proffer scientific, cultural sensitive solutions to the problems of substance abuse among Psychiatric patients. The following recommendations were suggested:
1. Immediate implementation of professional training and increase the funding for more research on substance abuse of psychiatry patients and also organizing sound orientation for the on the adverse effects of abusing substance. Lots of these orientation should be done on a platform which will be able to catch a wide number of people’s attention to desist from abusing substance. Although, the Nigeria society already have a constitution guiding against such behavior, but limited number of people have access to this constitution. Orientation should be done using the social media to curb these practice of substance abuse.
2. The people in the educational settings should develop a curriculum on substance abuse and its effect into some courses and subjects. Lack of awareness from onset is one of the factors which is making the abuse of substance more rampant. Changing this situation and perception will require institutionalizing curricula at medical, pharmacy as well as courses for individuals that focus on substance abuse and its related problem.
3. Increase and intensify one-on-one communication between patients and health care professionals about consequences of abusing substance. Organizing group and family therapies for patients and their significant others to educate and enlighten them on the steps and possible obstacles that they may encounter if those patients keep involving in abusing drugs. If these steps are adequately implemented. It is projected that there could be a 70 percent effectiveness rate of deduction in patient’s substance abuse behavior.
4. Government should legislate to discourage young adults from abusing substance, and even ensure implantation of the rule regarding the age of taking some drinks until an individual is mature enough to control his or herself. Lots of substances are sold in the environment very close to the inhabitation of these patients and these does not help in improving their health, hence, young adult focused enlightenment campaign on the negative consequences of substance is advocated.
Limitations
Just like most studies, this study has limitation as well. This study made use of survey design, which means that the study could not establish cause and effect relationship between predictor variables and the dependent variable used in the study. Also, self-report instruments were used to collect data and a major characteristics of self-report questionnaires is that they are prone to response or responder bias on the part of the patients who participated in this study. This inherent problem is common in research study of this nature whereby patients may provide socially acceptable responses. Limited patient recall may also encumber the outcome of this study, such that the category of patients engaged in this study (Psychiatric patients) may be limiting in mental capacities to provide intended responses. Another limiting factor is that the study was conducted in a single hospital where only two hundred and ten patients participated in the study, despite the plurality of the patients who visit the hospital from all walks of life. This situation may be limiting in that the results of the study may generalized with caution, holding into account issues such as cultural relativity of the multi-cultural and multi-ethnic composition of the Nigerian population. Future studies can leverage on this by conducting studies that represent the six geo-political zones of the Nigerian federation.
References
1. Ujumadu V (2022) 29.4m Nigerians abuse drugs –NDLEA. Vanguard Newspapers, June 29. Retrieved on 27/09/2022; accessed from:
2. Abdulkarim B (2005) A descriptive Epidemiology of Substance use and substance use disorders in Nigeria during the early 21st century. Drug Alcohol Dependence 91(1):1-9.
3. Abasiubong F, Bassey EA, Atting IA, Ekott JU (2008) A comparative study of knowledge and substance use in two secondary schools in Akwa Ibom State, Nigeria. Nigerian J Clinical Practice 11(1):45-51.
4. UNODC World Drug Report (2021) Pandemic effects ramp up drug risks, as youth underestimate cannabis dangers.
5. Kuussaari K, Karjalainen K, Niemela S (2020) Mental health problems among clients with substance use problems: A nationwide timeâ??trend study. Social Psychiatry Psychiat Epidemiol 55:507-516. 6. Barrett EL, Teesson M, Mills KL (2014) Associations between substance use, post-traumatic stress disorder and the perpetration of violence: A longitudinal investigation. Addictive Behaviour 39:1075-1080.
7. Danjuma A, Ibrahim A, Emmanuel A, Sunday O, Lateefah I (2016) Occurrence, pattern, and effects of nonconventional use of substances among youth in North-Central, Nigeria. World J Preventive Med 4(1):12-19.
8. World Health Organization (2021) Approaches to treatment of substance abuse. Programme on substance abuse. WHO.
9. Haladu AA (2003) Outreach strategies for curbing drug abuse among out-of-school youth in Nigeria: A challenge for community Based Organization (CBOS), in A. Garba (ed). Youth and drug abuse in Nigeria: Strategies for counselling, management and control. Kano: Matosa Press.
10. World Book Encyclopedia (2004) Chicago: World Book.
11. Gureje O, Degenhardt L, Olley B, Uwakwe R, Udofia O, et al. (2007) A descriptive Epidemiology of Substance use and substance use disorders in Nigeria during the early 21st century. Drug & Alcohol Depend 91(1):1-9.
12. Duru CB, Oluoha UR, Okafor CC, Diwe KC (2017) Sociodemographic determinants of psychoactive substance use among students of tertiary institutions in Imo State, Nigeria. J Addiction Resource Ther 8:345.
13. https://www.apa.org/pubs/highlights/ substanceuse#:~:text=Substance%20use%20disorder%20 encompasses%20varying,amphetamine%2C%20 cocaine)%3B%20and20more.
14. Adewuyi TDO, Akinsola EF (2013) Gender and peer influence on substance abuse among undergraduates in Lagos State University, Ojo, Lagos, Nigeria. Gender Behavior 11 (1):5342-5349.
15. Majekodunmi AB (2006) Psychoactive substance use among medical students in a Nigerian University, World Psychiatry 6(2):112-114.
16. Othman O, Liam Y (2014) On the relationship of irrational beliefs with mental health and academic performance of secondary school students (male and female) of Meshkinshahr, MA thesis (unpublished), Azad University, Science and Research Branch.
17. Okoye NN (2001) The adolescents and hard drugs: A psychological concern in R.U.N, Okonkwo & R.O. Okoye (eds). The Nigerian adolescent in perspective. A Publication of the Nigerian Society for Education.
18. Oshodi OY, Aina Kremer OF, Onajole AT (2010) Substance use among secondary school students in an urban setting in Nigeria: Prevalence and associated factors. African J Psychiatry 13(1):52-57.
19. Osinowo HO (2016) A promising baby in turbulent waters: Psychology, health care and the criminal justice system in Nigeria. An inaugural lecture (pp. 69-73), Ibadan: Ibadan University Press.
20. Adamson OE, Babalola D (2000) Relationship among achievement Motivation and Social Adjustment and Academic Performance of Nigerian. The Nigerian J Guidance Counselin, 7(1):130-141.
21. Roma P (1985) Social Adjustment Inventory. Pub; Agra Psychological Research Cell-Agra.
22. Nwakaego O (2013) Psychosocial dynamics of psychoactive substance misuse among Nigerian adolescents. Annals of African Med 3(3):111-115.
23. Skinner HA (1982) The drug Abuse Screening Test. Addict Behaviour 7(4):363-371.
24. Adama A (2013) Perception of drug abuse amongst Nigerian Undergraduates. World Journal of Medical Sciences, 1(2):133- 139.
25. Thakore S, Ismail Z, Jarvis S, Payne E, Rothenburg l (2009) The perceptions and habits of alcohol consumption and smoking among Canadian medical students. Academic Psychiatry 33(3):197-197.
26. Burke D (2011) The Tobacco Atlas. Geneva: World Health Organization.
27. Strawbridge W (2001) Religious attendance increases survival by improving and maintain good health behaviors, mental health and social relationships. Annual Behav Med 23:68-74.
28. Mpanza DM, Govender P, Voce,A (2022) Perspectives of service providers on aftercare service provision for persons with substance use disorders at a rural district in South-Africa. Subst Abuse Treat Prevention Policy, 17:60.
29. Oputeh M, (2015) Nigerian youth and drug abuse. Peer pressure and gender influence the response to risk information among alcohol using patients. 8-9.



