Research Article - (2024) Volume 9, Issue 12
Knowledge, Attitude and Practice of Market Women towards Papanicolaou Smear Screening in Abakaliki Metropolis
2Public Health, Alex Ekwueme Federal University Teaching Hospital, Abakaliki, Nigeria
3Otolaryngology-Head and Neck Surgery, Obafemi Awolowo University Teaching Hospital, Ife, Nigeria
4Medical Director, AMURT, Nigeria
5Glangwili Hospital, Wales, UK
Received Date: Nov 18, 2024 / Accepted Date: Dec 10, 2024 / Published Date: Dec 20, 2024
Abstract
Background: Cervical cancer is the second most common cancer among women worldwide and the most common cancer among women in developing countries including Nigeria. The estimated incidence in Nigeria is twenty-five out of a hundred thousand women. In most developing countries, poor public health awareness has contributed to the late diagnosis of the disease and poor clinical outcomes.
Aim: To assess the knowledge, attitude and practice of market women towards Papanicolaou smear screening in Abakaliki metropolis.
Method: A descriptive cross-sectional study
Result: The result showed that 42.48% of the 306 market women have heard about cervical cancer, and 46.85% of them (143 women) knew of cervical cancer screening. There was a fairly positive attitude towards pap smear screening as 69.28% of the 306 women said they would do the screening if made available. However, the practice was poor as only 4.93% (15 out of the 304 women) had done Pap smear screening for cervical cancer, all of whom were women with tertiary level of education. This study establishes that the Attitude was good as 69.28% agreed they would do the test. While the level of Knowledge of cervical cancer screening was poor (46.85%), the Practice was much poorer as only 4.93% of the respondents ever had cervical cancer screening.
Conclusion: There is good knowledge but poor attitude and practice of market women towards Papanicolaou Smear Screening in Abakaliki Metropolis. Public Health awareness and education must be encouraged and sustained to increase the utilisation of pap smear screening services at all levels of healthcare to enhance the prevention and/or diagnosis of cervical cancer especially among market women in Abakaliki Metropolis.
Keywords
Cervical, Cancer, Pap smear, Screening
Introduction
Cervical cancer is the second most common malignancy affecting women worldwide [1, 2]. It is the leading genital tract malignancy in developing nations. It is also the leading cause of cancer deaths among women in developing countries [1]. Out of the half a million women affected annually worldwide, nearly 250, 000 deaths are reported every year [2]. 80% of these women not only come from countries that control only 20% of the world’s cancer resources, but they also present for treatment late in which case only palliative measures can be offered to them [3, 4]. About 83% of the cases occur in developing countries, representing 15% of female cancers [5]. The incidence of cervical carcinoma in Africa is on the rise. Nonetheless, the true incidence of cervical cancer in many African countries is unknown as there is gross under-reporting. Very few countries have functioning cancer registries and recordkeeping is minimal or non-existent. Some of the figures 1-12, quoted in the literature are hospitalbased, which represents a small fraction of women dying from cervical cancer as most women cannot access hospital care and die at home [5]. Reported mortality rates in developed countries with successful screening programmes seldom exceed 5 per 100,000 women. The survival rate for cervical cancer patients in sub-Saharan Africa in 2002 was 21% compared with 70% and 66% in the United States and Western Europe respectively. In Nigeria where the majority of cases present in the late stages, it is the prevalent genital tract malignancy [6-8]. This genital tract malignancy is presently the only reproductive tract cancer that can be detected at an early stage before it becomes frankly invasive. The use of the Papanicolaou smear for screening the pre-invasive phase has been demonstrated to be helpful in early detection and cure of cervical cancer [9]. The fact that the organ in question is easily accessible and the symptoms of the disease could manifest early makes quick diagnosis and cure possible. Considering the public health significance and the magnitude of the disease several communities especially in the developed nations of the world adopted mass screening measures to prevent as well as reduce the burden of cervical cancer [4]. Some developed countries have made it a law through their parliament, making screening the right of women to live. The story is not the same in most developing countries where awareness is poor and several barriers against the utilisation of screening services exist.
In Nigeria like other developing nations, awareness and utilisation of screening services are not encouraging [5]. Even the opportunistic screening attitude of health workers in Nigeria is not widely practised by most reproductive health experts. Surprisingly, studies have shown that despite their knowledge of the disease and of the importance of screening amongst female health workers, utilisation of services is poor.
HPV is the primary etiologic agent of cervical cancer. There are over 100 types of HPV. The genital-type HPVs are divided into high, intermediate and low-risk types according to the association with genital tract cancer. High-risk types; HPV-16, -18, -31, and - 45 account for more than 90% of cervical carcinoma. HPV-16 is the most often found in Tanzania [11], and accounts for 41% of cervical malignancies. Transmission of HPV occurs primarily by sexual contact or by skin-to-skin contact [12]. Two viral oncoproteins, E6 and E7, of HPV-16 and HPV-18 are responsible for viral oncogenesis by destabilising two major cellular tumour suppressors- p53 and pRb respectively; as a consequence, the host cell accumulates more and more genetic (DNA) damage that cannot be repaired, leading to transformed cancerous cells [13]. The known predisposing factors for HPV infection and cervical cervix include early age at first sexual intercourse, multiple sexual partners, and a male consort who in turn has had intercourse with multiple women also confers a significant risk, smoking and in women who are immunosuppressed [14].
Primary prevention of cervical cancer aims at reducing the incidence of cervical cancer by controlling the causes and risk factors. Vaccines against HPV have been developed and provide effective protection against some HPV types. Two vaccines to prevent HPV infections, Gardasil and Cervarix are in the market. Gardasil is called quadrivalent as it protects against four types of HPV which are HPV-6, 11, 16 and 18. Cervarix is called a bivalent vaccine because it targets two HPV types: HPV-16 and 18 [15]. Gardasil and Cervarix are proven to be effective only if given before infection with HPV. Studies have shown that both Gardasil and Cervarix prevent nearly 100 per cent of the precancerous cervical cell changes caused by the types of HPV targeted by the vaccine up to four years after vaccination to women who were not infected at the time of vaccination [16]. Recommended ages are 9 to 25 [17, 18].
Other preventive measures include screening and treating premalignant cervical lesions. Limiting the number of sexual partners, avoiding or quitting smoking, minimising exposure to environmental tobacco, and consuming a diet rich in fresh vegetables and fruits may help reduce the risk of cervical cancer. Health promotion activities on sexual health, smoking cessation and a healthy diet can contribute to the prevention of cervical cancer. The largest gain in reducing cervical cancer incidence and mortality could be attained by increasing the coverage of women who are currently unscreened or screened only infrequently. For many years the Papanicolaou (Pap) smear has been the gold standard method of cervical cancer screening.
Problem Statement
Cervical cancer remains the second leading malignancy among women in Nigeria. It is therefore one of the most important public health diseases.
Studies in Africa and especially Sub-Saharan Africa indicate poor knowledge of women on cervical cancer as well as on screening for premalignant cervical lesions [19]. Screening has been shown to reduce the incidence of this malignancy in developed countries but in developing countries screening coverage is still low.
Rationale
Carcinoma of the cervix is a preventable disease; its prevention among other ways, is through the detection of premalignant stages of the disease, and treatment. In recent years, a screening test for cervical precancerous and cancerous lesions using visual inspection aided by acetic acid has been a suitable low-cost and feasible alternative modality for the control of cervical cancer in resource-poor settings. Detecting premalignant cervical lesions requires knowledge of the disease so that people are aware and have a positive attitude towards the screening for premalignant cervical lesions. Knowledge of the disease is important so that people are aware and through motivation they can have a positive attitude towards screening for premalignant cervical lesions. Not enough is known about the knowledge, attitude and practice of Nigerian women towards cervical carcinoma and screening for cervical lesions. This study aimed to assess the knowledge, attitude and practice of market women in Abakaliki metropolis towards Papanicolaou (pap)smear screening for cervical premalignant lesions which is key in preventing overt carcinoma of the cervix. Information obtained from this study is critical and would alert authorities so that proper measures can be taken to save the lives of Nigerian women by educating them and providing screening services in many places accessible to them. At the end of the study, education will be given to the study participants who had poor or no knowledge of pap smear screening, with the importance of screening particularly emphasized.
Research Question
Are the market women in Abakaliki metropolis knowledgeable about carcinoma of the cervix and screening for premalignant cervical lesions? What is the attitude and practice of these women towards Pap smear screening?
Purpose / Broad Objective
The purpose of this study is to examine the Knowledge, Attitude and Practice of market women in Abakaliki metropolis towards cervical Pap smear screening.
Objectives
The objectives of this study are to;
To determine the level of knowledge on cervical Pap smear screening among market women in Abakaliki metropolis.
Determine the attitude of market women in Abakaliki metropolis towards cervical cancer screening in the four markets studied.
Determine how the market women in Abakaliki metropolis in the studied markets practice Pap Smear screening.
Hypothesis
There is a significant relationship between profession and the practice of cervical Pap smear screening among market women in Abakaliki metropolis.
Literature Review
Only a few women in sub-Saharan Africa are ever screened for cervical cancer. Low levels of awareness and poor knowledge of cervical cancer coupled with the unavailability and inaccessibility of cervical cancer screening services are responsible for the small number of women being screened in sub-Saharan Africa and other developing countries. In developed countries, people seem to be aware of cancer and screening services are widely available and utilized. In a cross-sectional survey of 650 women 15-78 years of age randomly recruited in two hospitals in London, England, 76.2% perceived cervical cancer to be a common disease and there was good awareness of the association between this cancer with smoking and the number of sexual partners. Furthermore, 91.7% believed cervical cancer could be treated if detected early enough [20]. A study done in Malaysia on women aged 21- 56 years who had never had a Pap smear test, to explore their knowledge and awareness of cervical cancer and its screening, showed that there is a lack of knowledge on cervical cancer as well as a lack of knowledge on the Pap smear test [16]. Many women did not have a clear understanding of the meaning of an abnormal cervical smear and the need for the early detection of cervical cancer. Many believed that the purpose of the Pap smear test was to detect existing cervical cancer, leading to the belief that Pap smear screening is not required because the respondents had no symptoms. Despite considerable awareness of the link between cervical cancer and sexual activity, as well as the role of a sexually transmitted infection, none of the respondents had heard of the human papillomavirus [16]. In Kuwait, one study done regarding cervical cancer screening among Kuwaiti women found that the knowledge about the test was adequate in 147 (52.3%) women [19]. In Africa, a study done in Cameroon to assess the knowledge of cervical cancer by women living in Maroua, the capital of the Far North Province of Cameroon showed that of 171 women studied, only 48 (28%) had prior knowledge of cervical cancer [21]. A cross-sectional survey among college women in a university in Ghana showed that only 7.9% were aware of the link between human papillomavirus and cervical cancer [22]. Knowledge is also poor among health professionals in Niger where a survey of 144 female health professionals at two referral hospitals with facilities for Pap smears showed that twenty-two per cent could not list any risk factor for cervical carcinoma [23]. Practice towards screening for cervical carcinoma is poor to even those with knowledge of the disease and knowledge on the importance of screening. In developed countries, majority of the women went for screening as compared to developing countries. In a cross-sectional survey of 650 women aged 15-78 years randomly recruited at 2 hospitals in London, England, 80.5% of these women had had at least one Pap smear screening and 71.5% reported regular smears (every 3-5 years) [20]. Practice on screening among Africans was also shown to be poor as demonstrated in a study done in South Africa, despite knowledge of cervical cancer screening and the availability of such services, the majority of women (87%) from higher social and educational backgrounds did not undergo cervical screening. Most patients resided within a 12-kilometre radius of a facility that either provided or could potentially provide screening [24]. In one study in Nigeria where 144 questionnaires were filled only 5.7% had ever undergone a pap smear [25]. Some of the barriers to screening were embarrassment and pain. Others were psychological fear (36.8%), physiological pain (30.2%) and worry of family misunderstandings (some husbands were against it) (15.3%) which were considered the most dreadful situations by primary school teachers who had fears of having cancer in Taiwan [25, 26]. In sub-Saharan Africa, knowledge and awareness of cervical cancer and screening are poor and mortality is very high [27]. Tanzania reported poor knowledge of the disease in a study done among female inpatients at Muhimbili between August 1999 and January 2000. It was a case-control study to assess knowledge of cervical cancer symptomatology where the knowledge ranged between 30 and 50% among cases and controls respectively. Many patients thought the symptoms were due to bewitchment, husbands’ extramarital affairs, or husbands making love to their daughters. This study also showed that more than 90% of patients presented with invasive cervical cancer [28].
A study conducted on the perception of risk and barriers to cervical cancer screening at Moi Teaching and Referral Hospital, Edirch Kenya, revealed that of the 219 women interviewed, 12.3% of participants had a screening before, while 22.8% felt that they were at risk of cervical cancer, 65% of participants nevertheless wished to be screened [29]. A study on cervical cancer attitudes and beliefs in a Cape Town community showed that more than half of the participants never had a pap smear or had one more than ten years in the past. One-third did not know what a pap smear screening was. Lengthy waits and fatalistic beliefs also affected screening behaviour. Ethnicity was associated with differences in beliefs [30]. Another study was conducted on knowledge, attitudes and practice of cervical cancer screening among medical workers of Mulago Hospital, Uganda with a response rate of 92% (285). Of these, 93% considered cancer of the cervix a public health problem and knowledge about pap smear was 83% among. Less than 50% knew the risk factors for cervical cancer eligibility for screening interval of the females 65% didn’t feel susceptible to cervical cancer and 81% had never been screened. Only 26% had partners who had ever been screened. Only 14% of the final-year medical students felt skilled enough to use a vaginal speculum and 87% had never performed a pap smear [31]. A study on awareness of cervical cancer screening amongst students of health science at the University of Kebangsaan, Malaysia [32] showed a significant association between grade of knowledge and year of education (P<0.01). ANOVA test showed a highly significant correlation between mean score and year of education (P<0.001). There was a significant association between the grade of knowledge and the different programmes P = (0.003). There was also a significant association of mean score with races (P=0.004) and faculties (P=0.048) for the knowledge of prevention. A year of education showed significant correlation with grade of knowledge (P=0.001) and with median score (P=0.005) significant correlation between grade of knowledge and median score also existed for race (P=0.010) and P=0.013 respectively. On awareness and source of information, 85% were aware of cervical cancer while the remaining 15% were not. Mass media was the most popular source of information for the respondents (59.1%), followed by education (48.6%) and posters on university campuses (39.4%). On Attitude, there is no significant correlation between attitude and faculties (P=0.315) and year of education (P=0.749) [32]. In a study on cervical cancer and pap smear screening in Botswana [33], knowledge and perception showed that knowledge of cervical cancer and pap smear tests was inadequate among women with low incomes of the 18 women who had at least one pap smear test in their lifetime, eight (44%) had opportunistic testing as a result of having gynaecological symptoms, twelve (40%) had never had a pap smear screening test. Major barriers to pap smear screening included inadequate knowledge about pap smear testing, provider’s negative attitudes and limited access to doctors [33]. In Tanzania, a study on knowledge of cervical cancer and screening practices of nurses at a regional hospital revealed that less than half of the nurses had adequate knowledge regarding cervical cancer. There was a significant association between knowledge of cervical cancer and age. Knowledge was more adequate among the young nurses (P=0.027) and knowledge differed significantly between cadres. Registered nurses had more adequate knowledge than enrolled nurses (P=0.006) [34].
In Nigeria, a study of the knowledge, practice and screening for cervical cancer among female students of tertiary institutions in South Eastern Nigeria showed that out of the 220 students involved in the study, 60.9% of the students had knowledge of cervical cancer and about two-thirds (2/3) did not know about pap smear. This low participation in screening was attributed to several reasons including ignorance of the existence of such a test, lack of awareness of centres where such services are obtainable, ignorance of the importance of screening and the risk factors of cervical cancer [35]. Another study on knowledge, attitudes and practices of cervical cancer screening among urban and rural Nigerian women showed that only 15.5% of the respondents were aware of the availability of cervical cancer screening services, the awareness varies with the level of education (P<0.0001). About 4.2% had ever done a pap smear test and all were referred for screening. The most important factor hindering the use of available cervical cancer screening services was a lack of knowledge (49.8%) and the feeling that they had no medical problems or symptoms to bother about (32.0%) [36]. A study of cervical cancer screening among nurses at Lagos University Teaching Hospital showed that 92% of respondents were aware of the causative organisms of cervical cancer (Papillomaviruses). The major sources of information were the electronic media (43.9%) and health professionals (37.4%). 91% of respondents were aware of pap smear as a screening technique and had a good attitude (89%), but 75% of them had never done it before. The study showed that most respondents had good knowledge of cervical cancer but limited knowledge of the types of cervical cancer screening techniques [37]. A survey of Gynaecological cancer in Zaria, Northern Nigeria revealed that carcinoma of the cervix accounted for 66.7% of histologically confirmed gynaecological cancers [31]. The highest incidence was also observed in Maiduguri, NorthEastern Nigeria with 72.6% of Gynaecological cancers [32]. A high incidence was also recorded in Ibadan, South-West, Nigeria with 62.7% [4]. Another study in Ibadan by Ayinde et al. [38] on awareness and utilization of cancer screening among female undergraduates showed that the percentage of sexually active respondents was 81.5%. 57% had multiple sexual partners but 38.1% used condoms. 70% were aware of cervical cancer while 23.5% were aware of Papanicolaou smear. Awareness was found to be more common among medical students and the married ones. A study among female health workers in Ilorin [39] showed that 337 (69.8%) knew about pap smear as a screening procedure for cervical cancer while 146 (30.2%) had no such knowledge [39]. The commonest sources of information about pap smears were school lecturers (35.3%), textbooks (25.2%) and medical journals (10.7%).
Another study in Sokoto found that knowledge about cervical cancer screening was high among female health workers [40]. In Nnewi, Udigwe surveyed female nurses and that 122 (87%) were aware of the existence of screening services, although, 9.3% had lost relations to cervical cancer [41]. A study in Aba on the awareness and risk factors [4] showed that the majority of respondents were married (92%) and sexually active have initiated sexual activity at a young age (17.3 ± 2.5 years). There was a high prevalence of the major risk factors for cervical cancer. This includes initiation of coitus before 19 years (43.5%), multiple sexual partners (63.5%) and male partners with other female partners (2.5%). Also, a previous history of sexually transmitted disease (58.5%) and vulval warts (48%). Their overall role of cervical cancer was low and only 32 women (16%) had any knowledge of pap smear screening services. Also, there was poor appreciation of personal risk of cervical cancer and safer sexual practice [3]. In the research carried out by James Vasumu Jacob [42] between 2010-2011 on the Knowledge, Attitude and Practice concerning cervical cancer screening among market women in Yola-metropolis, Adamawa, among the 74.0% of market women who have heard about cervical cancer, 74.9% of them had also heard about the screening. Generally, there was a positive attitude toward cervical cancer screening (92%) with the majority having an attitude score of 19-25. While the majority (86.2%) of the women interviewed in the study admitted that cervical cancer screening was important for every woman, 87.0% of the women were willing to avail themselves of screening. Also, the majority (81.4%) of the respondents agreed that cervical cancer screening is beneficial and 90.5% of the respondents in the study were willing to advise their friends and relatives to go for cervical screening. The majority (51.2%) of the women who had ever been screened for cervical cancer were between the age of 16-20 years. 38.5% of those who had tested were 41-45 years of age. Only 21.3% of the women between 26- 30 years had ever tested for cervical cancer screening and the association was not statistically significant (p>0.05). More women with formal education (36.0% for primary and 31.3% for secondary) had taken up cervical cancer screening than those without formal education (20.6%) [42]. In a research on the Knowledge, Attitude and Utilisation of cervical cancer screening among 260 market women, aged 15 years and above, in Sabon Gari Local Government Area of Kaduna State [43], it was found that their knowledge of risk factors for cervical cancer was generally poor. However, 62.5% of them were aware that sexually transmitted infections were a risk factor.
Although their knowledge of symptoms of cervical cancer was fair, their attitude towards cervical cancer screening was poor (19.6%). Some patients would go to seek care after noticing symptoms in hospitals (72.1%), traditional healers (10.5%), and religious healers (7.4%), while 10.1% would not go anywhere. Many (32.7%) of the women had never heard of cervical cancer screening before, but 32.7% of others had been screened for cervical cancer. Of those who had been screened, 80.6% did so voluntarily while 68.2% were advised by friends or relations to take up cervical cancer screening. Respondents identified fear of screening outcome, lack of information and public awareness, lack of health worker requests, high cost of screening and lack of personnel at the screening centres as the reasons people do not patronise cervical screening [43].
Methodology
Study Area
The study was carried out in 4 markets within abakaliki metropolis in Ebonyi State which is located in the Eastern Nigeria. Abakaliki metropolis constitutes two local government areas, the Ebonyi and Abakaliki Local Government Areas. The four markets include Abakpa and Kpirikpiri markets which are located in Ebonyi local government area, and Nkwegu and Rice Mill markets which are located in Abakaliki local government area.
Study Design and Population
This cross-sectional study was carried out between July 2017 to February 2018 among the market women in Abakaliki metropolis from the age of 15 years and above. The market women involved those within the age bracket as stated above who buy and sell within the markets while those outside the age bracket and those who refused to give consent were excluded. The total population of the market women in Abakaliki metropolis is estimated to be 1500 with the distribution as below (Table 1).

Table 1: The total population of the market women in Abakaliki metropolis
Sample Technique
To calculate the minimum sample size required for accuracy in estimating proportions, this formula is used
N = z^2pq/d^2
where N = the desired sample size which we are going to work on
Z = the standard normal deviation usually set as 1.96 which corresponds to a 95% confidence level.
P = the proportion of the target population of market women in Abakaliki metropolis.
Since there has been no such kind of work done before in Abakaliki metropolis, we decided to use the value of 50% = 0.5
d = Degree of accuracy we desire which is set at 0.05
q = 1-p therefore
n = Z2 pq/d2 =
1.96 × 1.96 × 0.5 × 0.5/(0.05×0.05)
= 384 market women
Since our population size is less than 10000, this implies we are going to use this formula
nf = n/(1+ n/N)
where
nf = sample size when the sample population is less than 10000
n = sample size
when sample population is greater than 10000 =
384 N = sample population = 1500
nf = n/(1+ n/N)
= 384/(1 + 384/1500)
= 306 using this value to get the population of women in each market will be (Table 2)
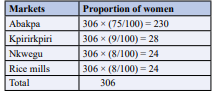
Table 2: 306 using this value to get the population of women in each market
Data Collection
In order to capture the whole area in the markets we are adopted a simple random sampling technique in the distribution of our questionnaires. We used both self-administered questionnaire and interviewer-based questionnaire methods depending on the level of academic qualification of the women involved. The questionnaire obtained information on the sociodemographic characteristics of the respondents, their knowledge, attitude and practice towards pap smear screening. The questionnaire was collected immediately after the person completed it
Data Analysis
This INFO version 7.0 software package was used for data validation and analysis.
Results
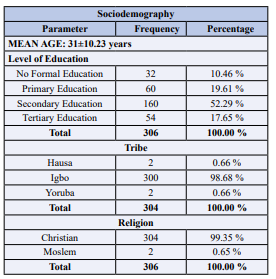
Table 3: The sociodemographic characteristics of the respondents, their knowledge, attitude and practice towards pap smear screening
The mean age of the study participants was 31±10.23 years. 19.9%of them were between the ages 26-30 years. The majority of the respondents (98.68%) were Igbo, while Hausa and Yoruba constituted 0.66% each. Most of them (99.35%) were Christians while only 0.65% were Muslims. The majority of them had secondary education (52.29%), 17.65% had tertiary education while the rest of them had primary or no formal education.
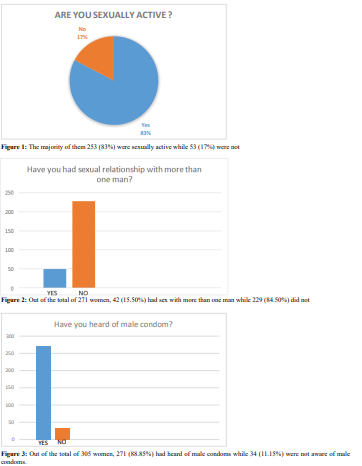
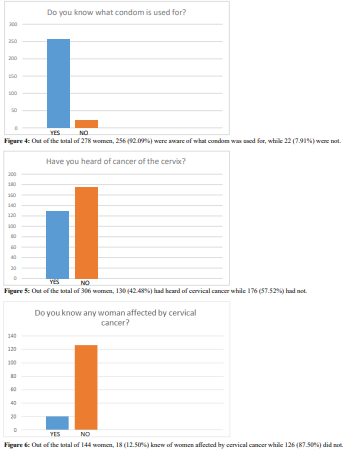
Discussion
The mean age of the respondents was 33±11.05 years. However, 19.8% of the market women involved in this study were between the ages of 26-30 years.
The majority of the women were Igbo (98.68%). A majority of them had secondary level of education (52.29%) while 10.46% had no formal education at all.
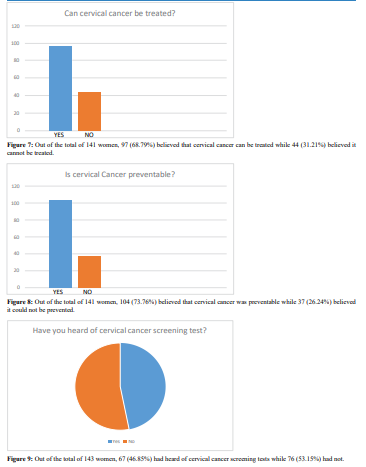
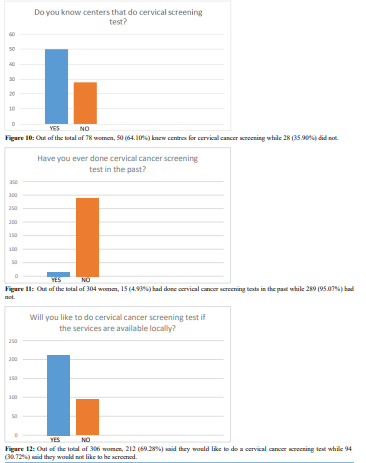
had no formal education at all. Christianity is the dominant religion practised by almost all (99.39%) of the women in this study. The above findings are similar to findings by other studies in Eastern Nigeria, 45 and 46 who have all reported similar distribution of these demographic characteristics. Among the 42.48% of the market women who have heard about cervical cancer, 46.85% of them had also heard about the Pap smear screening. This finding contrasts previous reports on the awareness of cervical cancer screening from earlier studies by Vasumu Jacob 48 among market women in Yola metropolis where 74.0% of the women were aware of cervical cancer out of which 74.9% knew about the screening services. Similar high awareness had been observed in the studies 45 involving female nurses in Nnewi which reported awareness of 87%, 43 which reported awareness of 69.8%, and 38 which reported 60.9% awareness of cervical cancer screening among females of tertiary colleges. However, the result of this study is similar to that of 39 which recorded 15.5% awareness among Urban Nigerian women, 46, Feyi-Waboso et al. in Aba, Abia State which showed 16% had heard of cervical cancer screening tests, Ayinde et al. 43 showed 23.5% awareness among female undergraduates and Saad Aliyu et al 48, which as well showed poor level of awareness of cervical cancer screening among market women in Sabon Gari LGA of Kaduna State. In this research, few of the women (17.09%) had sex with more than one man while 15.5% believed that their spouses had other sexual partners. These are also similar to the results of other works cited in this research. The attitude of the women in this study was fair, as 69.28% said they would agree to be screened if the facilities were made available while the rest (30.72%) said they believed they did not have and would not have the disease, hence would not go for the screening even if it was made available. This poor attitude contrasts that reported by James Vasumu [42], who recorded 92% willingness to do cervical cancer screening among market women in Yola metropolis and Awodele et al. [37] which recorded a positive attitude of 89% among female nurses in Lagos University Teaching Hospital. However, this poor attitude is similar to the findings of Fayemi-Waboso et al. [4] who reported a low attitude towards Pap smear screening and also that of Saad Aliyu et al. [43] who documented a low attitude of 19.6%. The Practice of the women in this study was grossly poor as only 4.93% had done screening for cervical cancer. This is in tandem with all of the similar research which recorded a low percentage of women who had been screened for cervical cancer.
Conclusion
The result showed that 42.48% of the 306 market women had heard about cervical cancer while 46.85% of 143 women knew about cervical cancer screening which demonstrates suboptimal knowledge. There was an optimal attitude as 69.28% of the 306 women said they would do the screening if made available.
However, the practice was very poor as only 4.93% (15 out of the 304 women) had done Pap smear screening for cervical cancer, all of whom were women with tertiary level of education. Recommendations.
There is need for a sustained public awareness of the benefits of cervical cancer screening as well as the location of screening centres.
The government at all levels should understand that cervical cancer is a serious public health challenge and throw in their support to ensure that its awareness by the public is high and that centres for cervical cancer screening and treatment are established across all the States and major cities in Nigeria with the cost subsidised if not made free.
Conflict of Interest Statement
The authors declare that there are no conflicts of interest.
Affiliate Institution:
Alex Ekwueme Federal University Teaching Hospital Abakaliki.
Funding Information
This work received no specific grant from any funding agency.
Ethical Approval
Ethical consent was obtained from the Research and Ethical committee of Alex Ekwueme Federal University Teaching Hospital Abakaliki with permission granted by the ministry of health Ebonyi State. Also informed consent was obtained from the market women before questionnaires were given to them to fill.
Consent for Publication
The consent for publication was obtained from all the contributing authors and the affiliate institution, the Alex Ekwueme Federal University Teaching Hospital Abakaliki.
Acknowledgment
The work does not receive any assistance from any laboratory or institution.
References
1. Kikelomo, A., Rakiya, S., Abiodun, A., Adegboyega, F., Adebunmi, O., I. K. (2009). Factors contributing to low uptake of cervical screening in a population at risk. Trop J Obstet Gynaecol, 26, 35-41.
2. Balogun, M. R., Odukoya, O. O., Oyediran, M. A., & Ujomu, P. I. (2012). Knowledge of cervical cancer and its risk factors among women residing in two urban slums in Lagos, Nigeria. Nigerian Medical Practitioner, 61(5), 74- 81.
3. Aboyeji, P. A., Ijaiya, M. D. A., & Jimoh, A. G. A. (2004). Knowledge, attitude and practice of cervical smear as a screening procedure for cervical cancer in Ilorin, Nigeria. Tropical journal of obstetrics and gynaecology, 21(2), 114.
4. Feyi-Waboso, P. A., Kamanu, C., & Aluka, C. (2005). Awareness and risk factors for cervical cancer among women in Aba, south-eastern Nigeria. Tropical Journal of Obstetrics and gynaecology, 22, 25-26.
5. Jemal, A., Thomas, A., Murray, T., & Thun, M. (2002). Cancer statistics, 2002. Ca-A Cancer Journal for Clinicians, 52(1), 23-47.
6. Roblyer, D., Park, S. Y., Richards-Kortum, R., Adewole, I., & Follen, M. (2007). Objective screening for cervical cancer in developing nations: lessons from Nigeria. Gynecologic Oncology, 107(1), S94-S97.
7. Anorlu, R. I. (2008). Cervical cancer: the sub-Saharan African perspective. Reproductive health matters, 16(32), 41-49.
8. Onah, H. E., Ezugwu, F. O., & Eze, J. N. (2001). Cervical cancer screening: A survey of current practice amongst Nigerian gynaecologists. Tropical Journal of Obstetrics and Gynaecology, 18(2), 78-81.
9. Chukwuali, L. I., Onuigbo, W. I., & Mgbor, N. C. (2003). Cervical Cancer Screening in Enugu, Nigeria. Tropical Journal of Obstetrics and Gynaecology, 20(2), 109-112.
10. Nwobodo, E. I., & Malami, S. A. (2005). Knowledge and practice of cervical screening among female health workers in Sokoto, North Western Nigeria. Nigerian Postgraduate Medical Journal, 12(4), 255-257.
11. Muñoz, N., Bosch, F. X., De Sanjosé, S., Herrero, R., Castellsagué, X., Shah, K. V., ... & Meijer, C. J. (2003). Epidemiologic classification of human papillomavirus types associated with cervical cancer. New England journal of medicine, 348(6), 518-527.
12. Walboomers, J. M., Jacobs, M. V., Manos, M. M., Bosch, F. X., Kummer, J. A., Shah, K. V., ... & Muñoz, N. (1999). Human papillomavirus is a necessary cause of invasive cervical cancer worldwide. The Journal of pathology, 189(1), 12-19.
13. Park, T. W., Fujiwara, H., & Wright, T. C. (1995). Molecular biology of cervical cancer and its precursors. Cancer, 76(S10), 1902-1913.
14. Emirates, U. A. (2004). The knowledge, attitude and practice of pap smear among local school teachers in Sharjah district. Middle East J Fam Med, 4, 10-18.
15. Koutsky, L. A., Ault, K. A., Wheeler, C. M., Brown, D. R., Barr, E., Alvarez, F. B., ... & Jansen, K. U. (2002). A controlled trial of a human papillomavirus type 16 vaccine. New England Journal of Medicine, 347(21), 1645-1651.
16. Wong, L. P., Wong, Y. L., Low, W. Y., Khoo, E. M., & Shuib, R. (2009). Knowledge and awareness of cervical cancer and screening among Malaysian women who have never had a Pap smear: a qualitative study. Singapore medical journal, 50(1), 49.
17. Garland, S. M., Hernandez-Avila, M., Wheeler, C. M., Perez, G., Harper, D. M., Leodolter, S., ... & Koutsky, L. A. (2007). Quadrivalent vaccine against human papillomavirus to prevent anogenital diseases. New England Journal of Medicine, 356(19), 1928-1943.
18. Paavonen, J., Naud, P., Salmerón, J., Wheeler, C. M., Chow, S. N., Apter, D., ... & Dubin, G. H. P. V. (2009). Efficacy of human papillomavirus (HPV)-16/18 AS04-adjuvanted vaccine against cervical infection and precancer caused by oncogenic HPV types (PATRICIA): final analysis of a double-blind, randomised study in young women. The Lancet, 374(9686), 301-314.
19. Al Sairafi, M., & Mohamed, F. A. (2008). Knowledge, attitudes, and practice related to cervical cancer screening among Kuwaiti women. Medical Principles and Practice, 18(1), 35-42.
20. Yu, C. K., & Rymer, J. (1998). Women’s attitudes to and awareness of smear testing and cervical cancer. The British journal of family planning, 23(4), 127-133.
21. Tebeu, P. M., Major, A. L., Rapiti, E., Petignat, P., Bouchardy, C., Sando, Z., ... & Mhawech-Fauceglia, P. (2008). The attitude and knowledge of cervical cancer by Cameroonian women; a clinical survey conducted in Maroua, the capital of Far North Province of Cameroon. International Journal of gynecologic cancer, 18(4).
22. Abotchie, P. N., & Shokar, N. K. (2009). Cervical cancer screening among college students in Ghana: knowledge and health beliefs. International Journal of Gynecologic Cancer, 19(3).
23. Anya, S. E., Oshi, D. C., Nwosu, S. O., & Anya, A. E. (2005). Knowledge, attitude, and practice of female health professionals regarding cervical cancer and pap-smear. Nigerian Journal of Medicine, 14(3), 283-286.
24. Wellensiek, N., Moodley, M., Moodley, J., & Nkwanyana, N. (2002). Knowledge of cervical cancer screening and use of cervical screening facilities among women from various socioeconomic backgrounds in Durban, Kwazulu Natal, South Africa. International Journal of Gynecologic Cancer, 12(4).
25. Udigwe, G. O. (2006). Knowledge, attitude and practice of cervical cancer screening (pap smear) among female nurses in Nnewi South Eastern Nigeria. Nigerian journal of clinical practice, 9(1), 40-43.
26. Yang, N. P., & Chou, P. (1991). The knowledge attitude and practice of cancer prevention among primary school teachers. Zhonghua yi xue za zhi= Chinese Medical Journal; Free China ed, 47(4), 271-279.
27. Gichangi, P., Estambale, B., Bwayo, J., Rogo, K., Ojwang, S., Opiyo, A., & Temmerman, M. (2003). Knowledge and practice about cervical cancer and Pap smear testing among patients at Kenyatta National Hospital, Nairobi, Kenya. International Journal of Gynecologic Cancer, 13(6).
28. Kidanto, H. L., Kilewo, C. D., & Moshiro, C. (2002). Cancer of the cervix: knowledge and attitudes of female patients admitted at Muhimbili National Hospital, Dar-es-Salaam. East African medical journal, 79(9), 467-475.
29. Airede, L. R., Nwobodo, E., Malami, S. A., & Tunau, K. (2005). Carcinoma of the cervix in Sokoto, Northern Nigeria. International Journal of Medicine and Health Development, 10(1), 48-52.
30. Reeler, A., Qiao, Y., Dare, L., Li, J., Zhang, A. L., & Saba, J. (2009). Women’s cancers in developing countries: from research to an integrated health systems approach. Asian Pac J Cancer Prev, 10(3), 519-526.
31. Sadjadi, A., Malekzadeh, R., Derakhshan, M. H., Sepehr, A., Nouraie, M., Sotoudeh, M., ... & Alimohammadian, M. (2003). Cancer occurrence in Ardabil: Results of a populationâ?based Cancer Registry from Iran. International journal of cancer, 107(1), 113-118.
32. Jedy-Agba, E., & Adebamowo, C. (2012). Knowledge, attitudes and practices of AIDS associated malignancies among people living with HIV in Nigeria. Infectious Agents and Cancer, 7, 1-8.
33. Ferlay, J., Shin, H. R., Bray, F., Forman, D., Mathers, C., & Parkin, D. M. (2010). Estimates of worldwide burden of cancer in 2008: GLOBOCAN 2008. International journal of cancer, 127(12), 2893-2917.
34. Sankaranarayanan, R., Budukh, A. M., & Rajkumar, R. (2001). Effective screening programmes for cervical cancer in low-and middle-income developing countries. Bulletin of the World Health Organization, 79(10), 954-962.
35. Jemal, A., Siegel, R., Ward, E., Hao, Y., Xu, J., & Thun, M. J. (2009). Cancer statistics, 2009. CA: a cancer journal for clinicians, 59(4), 225-249.
36. Ries, L.A.G., Eisner, M.P., Kosary, C.L., Hankey, B.F., Miller, B.A., Clegg, L., et al. (2005). SEER Cancer Statistics Review, 1975-2002. National Cancer Institute 2005.
37. Awodele, O., Adeyomoye, A. A., Awodele, D. F., Kwashi, V., Awodele, I. O., & Dolapo, D. C. (2011). A study on cervical cancer screening amongst nurses in Lagos University Teaching Hospital, Lagos, Nigeria. Journal of cancer education : the official journal of the American Association for Cancer Education, 26(3), 497–504.
38. Ayinde, O. A., Omigbodun, A. O., & Ilesanmi, A. O. (2004). Awareness of cervical cancer, Papanicolaou’s smear and its utilisation among female undergraduates in Ibadan. African Journal of Reproductive Health, 68-80.
39. Sant, M., Aareleid, T., Berrino, F., Lasota, M. B., Carli, P. M., Faivre, J., ... & EUROCARE Working Group. (2003). EUROCARE-3: survival of cancer patients diagnosed 1990–94—results and commentary. Annals of Oncology, 14, v61-v118.
40. Bailie, R., Pick, W., & Cooper, D. (1996). Cervical cytology screening-knowledge, attitudes and practice in a periurban settlement. South African Medical Journal, 86(9).
41. Eddy D. M. (1986). Secondary prevention of cancer: an overview. Bulletin of the World Health Organization, 64(3), 421–429.
42. Jacob, J.V. (2014). Knowledge, Attitude and Practice concerning cervical cancer screening among market women in Yola-metropolis, Adamawa 2010- 2011. Almadu Bello University. 2014.
43. Ahmed, S. A., Sabitu, K., Idris, S. H., & Ahmed, R. (2013). Knowledge, attitude and practice of cervical cancer screening among market women in Zaria, Nigeria. Nigerian Medical Journal, 54(5), 316-319.
Copyright: © 2025 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.



